Brief description
- Your child is going to be having a pH-impedance study. This information leaflet will provide you with the information you need about this procedure.
- Here, we explain some of the aims, benefits, risks and alternatives to this procedure. We want you to be informed about your choices to help you to be fully involved in making any decisions.
- Please ask about anything you do not fully understand or wish to have explained in more detail.
What is a pH-Impedance study?
This test measures the movement of all liquid and air up and down the oesophagus (the food pipe - the tube that takes food from your mouth to your stomach). Gastro-oesophageal reflux (GOR) is when stomach content (acid or non-acid) comes back up from the stomach into your oesophagus. The impedance study provides information on what is actually happening in the oesophagus over 24 hours. It measures all reflux events, whether they are acid or non-acid, liquid or air, or liquid and air combined. It also measures how high the liquid refluxes, for example, into the lower, middle or upper part of the oesophagus. These events are measured using a pH-impedance probe.
What are the benefits of this procedure?
Your doctor should have discussed the likely benefits of this procedure with you and your child. If you are not sure how the procedure is likely to benefit your child’s health, please ask one of the medical team who will be happy to explain this to you.
In most cases the procedure is done to try and help make a diagnosis, that is to say to work out the cause of your child’s symptoms and therefore allow better treatment for your child.
Alternatives
Some units measure pH reflux alone with a ‘pH-study’. A pH-impedance study is a better study of the function of the oesophagus and cannot be replaced by any other type of scan/ x-ray or blood test. Sometimes it is appropriate to treat a patient without doing an impedance study, but this should be discussed with you before booking this investigation.
Preparation - what to do with medication?
Before booking the study your doctor or specialist nurse will discuss with you whether or not you need to stop any of your child’s treatment.
Occasionally the doctor caring for your child may request that you do not stop their medication; they will explain to you why this is important.
If your child needs to stop treatment, then please see the list below for when these should be stopped.
Proton pump inhibitors should be stopped seven days before the test. These include:
- Omeprazole (Losec)
- Lansoprazole (Zoton)
- Esomeprazole (Nexium)
Other medications that should be stopped for 72 hours (three days) before the test include:
- Ranitidine (Zantac)
- Cimetidine
- Famotidine
- Nizatidine
- Domperid
- Gaviscon
- Gastrocote
- Peptac
- Rennies
- Maalox
- Mucogel
- Prokinetic (motility agents)
- Domperidone (Motilium)
Before the test
You will receive information regarding the date, time and department where your child will have the test performed.
Your child should not eat or drink for two hours before this appointment to reduce the chance of them being sick at the time of probe insertion.
How is the probe inserted?
Before inserting the probe, the specialist nurse will talk your child through the procedure. If your child is not having an endoscopy/ bronchoscopy, the specialist nurse will pass the tip of a very thin flexible plastic tube (called a probe) into your child’s nose and down the back of their throat into the lower oesophagus.
This is a little uncomfortable and may make your child sneeze, cough or retch. It may tickle the back of their throat for a while once inserted. The probe is held in place with tape attached to your child's cheek and is also secured with tape on the back or chest. The other end of the probe is attached to the recording box, which is the size of a Nintendo DS and held in a small bag. The box will record the severity of acid reflux (pH) and any reflux (impedance) events over 24 hours. The data is later transferred onto a computer for analysis. The test will then be analysed by your child’s medical team and appropriate changes made to their treatment plan.
Is the probe in the correct position?
The majority of patients will have the impedance probe inserted during endoscopy, so the position is confirmed by direct vision of the Consultant. However, if you are having the probe inserted at the bedside, you will need to have an x-ray to be performed to ensure the probe is in the correct place. If necessary the probe can be pushed in slightly or pulled back to the required position. A further x-ray is not needed.
Will my child need to stay in hospital?
In most cases it is possible for your child to go home overnight and return to the ward the following day for the probe to be removed. This will be discussed with you by your child’s team. If your child remains in hospital overnight they will be nursed on a children’s ward.
How will the probe stay in?
The probe will be secured to your child’s nose/ cheek and back or chest with tape to avoid accidental removal. You will be shown how to re-secure the probe if the tape becomes loose.
Will my child feel the probe?
Your child will be aware of the probe in the back of their throat throughout the test but most children/ young people report they become less aware of it over the 24 hour period.
What happens if the probe falls out?
This is very uncommon. If the probe does fall out, don’t worry! If you are in hospital, tell one of the nursing staff immediately and they can contact the nurse specialist as appropriate. If you are at home and the probe falls out, simply remove it by pulling it out of the nose gently. If it comes out slightly, you can try to return it to its original position. If this is not easily done, either fix the tube in the new position (please inform the nurse specialist by phone or when you return to the ward) or simply remove the tube and return to the ward the next day as planned.
What should I do if my child cannot tolerate the presence of the probe?
This is very rare, but children who cannot tolerate the probe are usually identified at the time of insertion. If you find that your child really cannot tolerate the probe when you get home, and that simple pain relief (for example paracetamol) does not help, you can remove the probe yourself by simply removing the tape and pulling out the probe. If you do remove the probe please remember to take the battery out of the recorder.
Return the recorder and probe to the hospital as planned the next day and explain what happened to your nurse specialist.
Will my child be able to eat and drink as normal?
We want your child to continue eating and drinking as normal, as we need to see what happens during a normal day. However, we ask that your child does not have any carbonated/ fizzy drinks or fruit juices during the study as these can interfere with the interpretation of reflux events. The probe may move very slightly as your child eats, and this may feel strange initially. This is perfectly normal.
Are there any restrictions to my child's activities?
Your child should not have a bath or shower for the duration of the study to prevent any accidental damage to the recorder by water.
Boisterous play/activity or sandpits are best avoided to prevent accidental removal of the probe and damage to the recorder.
How will my child sleep?
Your child will be able to sleep as normal. Place the recorder/box under your child’s pillow to avoid accidental removal. If your child’s sleep is disturbed overnight, press the appropriate button, as advised. Ensure the probe is secured so as to prevent it becoming entangled around your child.
What happens when the monitoring is complete?
Please ensure that you return the box along with the black satchel at least 24 hours after your child had the probe placed. You will be told to go to Ward F3 to have the probe removed and where the box can be returned by a member of the gastroenterology team.
The appointment to remove the probe will take 10 to 15 minutes. Once the tape is removed the probe slips out of the nose very easily. This only takes a few seconds and may feel odd, but it should not be painful. Each probe is only ever used once and then discarded.
Once the probe is out your child can go home. Any anti-reflux medication can be restarted if this was advised by your doctor before the study.
Your impedance monitoring box user guide

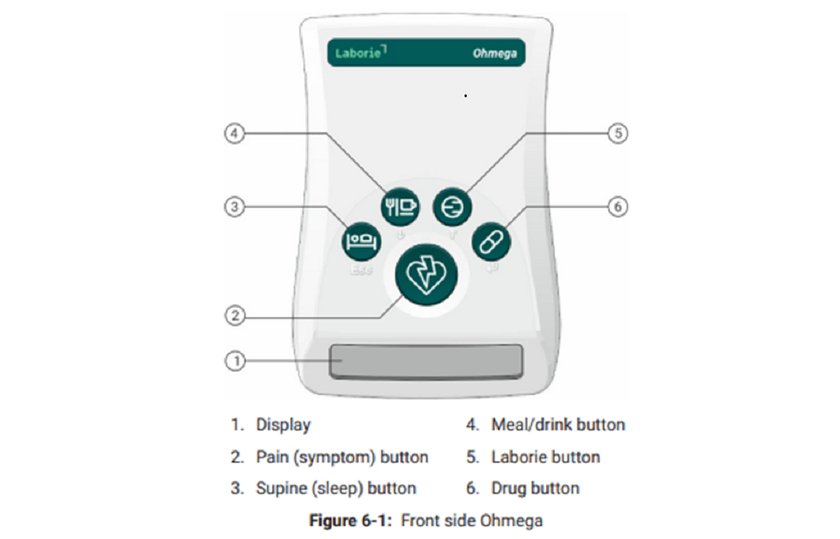
Operation functions
- Display Screen - This screen displays the pH level in the top right corner, and has your name below it
- Pain Symptom Button – Press this button whenever you experience pain - related to impedance study symptoms.
- Sleep (Supine) Button – Press this button each time you lie down and when you sit back up.
- Meal and Drink Button – Press this button at the start of eating and drinking, and press it again once you have finished.
- Laborie Button – This button does not need to be pressed by the patient.
- Drug Button – Press this button whenever you take any medication.
When do I find out the results?
The information on the Impedance recorder is downloaded onto a computer and the results are analysed by the doctor or specialist nurse from your child’s team. This can take approximately two weeks but may be longer and you will either receive a telephone call or be seen in clinic to discuss the results.
A letter confirming the findings of the procedure and management plan will be given to you, your child’s GP, your referring consultant and any other healthcare professionals involved in your child’s care. If you do not wish for anyone involved in your child’s care to receive this information, please let one of the team know.
Are there any risks?
There may be a little bleeding from the nose if your child has a history of nosebleeds, or the tube was difficult to insert.
There is also a small risk of the probe going into a lung rather than the oesophagus. This is very uncommon and not dangerous. Misplacing the probe is very unlikely as passing the probe into the lungs will usually make your child continue to cough and feel uncomfortable.
If having a bedside insertion, you will need to have an x-ray to confirm the correct position of the probe. before your child is allowed to eat, drink or leave the hospital.
Approximately 1 in 20 patients may experience a probe malfunction.
Do not carry or use a mobile phone during a measurement, as this may affect the monitor reading.
Do not have the monitor within the immediate area of a FM radio.
Troubleshooting
There may be the odd occasion when your impedance box is not recording. Here are some tips on what to do if that should happen:
The box will give a pH Value in the top right hand corner when recording. This number should change through the course of the study; if this is not the case the box may be in standby mode: press the power button to resume.
If the screen goes blank altogether, this may mean that the battery needs replacing. The box takes one AA battery and this is inserted at the back of the box. Press the pain button in the middle to resume the recording.
There is no on/off button; the only way to stop the study is to remove the battery.
Occasionally, there can be a technical failure with the recorder resulting in it being unable to proceed with the study or no data being collected. In these circumstances it will be discussed with you as to whether the procedure is rescheduled.
- You should avoid extreme temperatures, pressures, humidity and dust.
- You should ensure to keep pets away from the monitor and the probe to minimise any damage to the monitor.
- Parents need to watch their child closely whilst they are connected to the impedance study.
- Any questions at all please call Ward F3 on 01223 217569.
Can the equipment be damaged?
Yes. The equipment is very fragile and expensive. We therefore ask you and your child to take great care of it. The recorder should be handled carefully and kept in its case to avoid any accidental damage. If the equipment is damaged we will not be able to analyse the information of the test and the test may need to be repeated.
If you are concerned, or if your child has any of the symptoms below:
- Severe pain
- Fever – temperature higher than 38.5°C for more than two hours
Please contact one of the following:
- 08:00 until 16:00: gastroenterology nurse: 01223 348950
- 16:00 until 08:00: Your GP or local Accident and Emergency Department or;
- Addenbrooke’s Hospital Contact Centre: 01223 245151 (ask for the on-call paediatric registrar to be bleeped).
Any other questions?
Feel free to write down any other questions you may have. No question is ever too minor or too silly to ask, so please ask any member of the team caring for you if there is anything you wish to know. Your child is also encouraged to ask questions. It is important that you and your child are fully prepared for the procedure. We will try to address all of your worries and concerns before the procedure.
If you have any problem understanding or reading any of this information, please contact any of the team below or ask your consultant for more details.
- Clinical nurse specialists in paediatric gastroenterology: 01223 348950
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

