This leaflet explains what a nerve block is, how it is given, what to expect before, during and after your surgery, and the possible risks. It is designed to help you understand your anaesthetic options and to support shared decision-making with your anaesthetist.
This leaflet explains:
- What a nerve block is
- Why you could benefit from having one for your operation
- How is the nerve block performed?
- What happens after and how do you look after my numb arm till the block wears off
- Risks and shared decision-making.
What is a Brachial Plexus Block?
A nerve block is an injection of local anaesthetic (numbing solution) around specific nerves to temporarily stop pain and sensation in a particular area of the body. For arm and hand surgery, the anaesthetic is injected around the brachial plexus which is a network of nerves between the neck and armpit that controls movement and feeling in the arm. After the injection, the arm will feel warm, heavy, and numb, and while pain is blocked, you may still feel some pressure or movement. The numbness usually lasts up to 24 hours and occasionally up to 48 hours.

Benefits
Choosing a nerve block as part of your anaesthetic offers several benefits, including better pain relief, faster recovery, less nausea, and a reduced risk of blood clots. Avoiding the risks and side effects of general anaesthesia such as sickness, drowsiness, and sore throat; particularly useful for patients with heart or breathing problems. When used alongside a general anaesthetic, a brachial plexus block provides excellent postoperative pain relief for 12–24 hours, reducing the need for strong painkillers and helping physiotherapists begin early movement to aid recovery.
How is the nerve block is preformed?
In theatre / block room, your anaesthetist and assistant will confirm the operation site, insert a small cannula for fluids and medication, and start routine monitoring. The local anaesthetic injection (nerve block) is performed under ultrasound &/or nerve stimulator guidance, with the injection site depending on the operation: neck, armpit, collarbone, or further down the arm. The area is numbed with a small sting, and you may feel tingling or twitching as the nerves are located. The block takes 20–40 minutes to work, during which your arm becomes warm, heavy, and numb. Your anaesthetist will ensure the block is effective before skin incision and that you remain comfortable throughout.
If the block is incomplete, rescue block could be performed to cover the spared nerve or offer a general anaesthetic.
During your operation
A screen will be positioned in a way that you cannot see the surgery being done. You may be able to listen to your own music on your own device with headphones during the surgery (please ask if this is possible).
If you are having sedation, you will be relaxed and drowsy. You may be given oxygen through a light plastic facemask. You may have memories of being in the operating theatre, although these may be patchy.

After your operation
Following the operation, you may return from the operating theatre with a sling or temporary splint to keep your arm protected as long as it is still numb.
Your anaesthetist may be able to give you an idea of how long it should take
before the block to wear off. As the block wears off you may begin to feel more discomfort, although by this time a lot of the inflammation and swelling from the surgery should have subsided. Regular pain killers will be prescribed to be taken for few days and strong opiate as a rescue pain killer if needed.
Aftercare at home
Your arm might still be numb when you return home from hospital as a result you will not be fully aware where your arm is and so it can be easily injured.
You should keep your arm in the sling you are given for support and protection. Take special care around heat sources, such as fires or radiators. You will not feel heat while your arm is numb and you may burn yourself. Avoid using your arm for strenuous or heavy tasks
If the block has not fully worn off two days after the operation you should contact your anaesthetist by calling the number given on your discharge paperwork.

Side effects, complications and risks
In modern anaesthesia, serious problems are uncommon, but risk cannot be removed completely. Modern drugs, equipment and training have made anaesthesia a much safer procedure in recent years.
People vary in how they interpret words and numbers. This scale is provided to help.
Anaesthetists take a lot of care to avoid all the risks given in this section. Your anaesthetist will be able to give you more information about any of these risks and the precautions taken to avoid them.
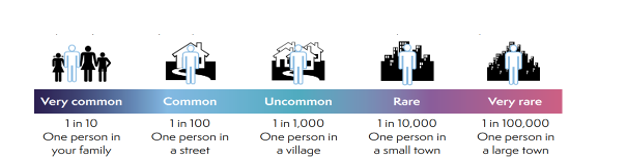
Risk due to local anaesthetic drugs
- Allergy to local anaesthetics.
- Another rare side effect an overdose of the local anaesthetic (serious problems including fits, heart or breathing problems), but should not happen because your weight is taken into account when choosing how much local anaesthetic you need and your anaesthetist is trained to manage these emergencies safely.
Risk to nearby structures
Side effects depend on where the nerve block is performed. When the injection is given in the side of the neck (for shoulder surgery), temporary effects may include a hoarse voice, droopy eyelid, light-headedness, or mild breathing difficulty, all of which resolve as the block wears off. For blocks around the collarbone (used for upper arm or elbow surgery), there is a small risk of lung injury (about 1 in 1000), which is usually safely managed with serious complications being very rare. At all injection sites, there is also a small risk of bleeding from a blood vessel, typically controlled with pressure or intravenous fluids.
Nerve damage
Nerve damage can occur because of direct injection into the nerve or because of bleeding or infection. The risk of permanent nerve damage is rare. An exact measure of the risk is not available, but the best studies we have suggest that it happens between 2-5 in 10,000.
There is a risk of nerve damage after any operation regardless of the type of anaesthetic technique used. This can be due to the operation, the position you lie in or the use of a tourniquet (a tight band on the upper arm, which prevents bleeding during the operation). Swelling around the operation site or a pre-existing medical condition, such as diabetes, may also contribute to nerve damage.
References
- Neal JM et al Brachial Plexus Anaesthesia: Essentials of our current understanding. Regional Anaesthesia and Pain Medicine 2002; 27(4): 402-8
- Borgeat A, Ekatodramis G, Kalberer F, Benz C. Acute and non-acute complications associated with inter-scalene brachial plexus block and shoulder surgery; a prospective study. Anesthesiology2001; 95: 875-880
- Saha S, Turner J. Nerve damage associated with peripheral nerve blockade. Royal College of Anaesthetists, patient information leaflets.
If you would like to watch a more detailed and explanatory video, please scan the QR code below. The video will guide you through an informative journey about nerve blocks.
RA UK Nerve Blocks: An Information Video For Patients.

We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

