The Wolfson Diabetes and Endocrine Clinic
This booklet has been written to provide you with the information you need when using a Medtronic 740G or 780G insulin pump without continuous glucose monitoring (CGM). Please refer to the additional closed loop supplement if using a 780G with CGM.
Medtronic contact number
- Telephone: 01923 205167 option 2 technical support
Please note that the pump companies will not give medical advice and can only offer technical support if you are having problems with the pump.
Key points
When using an insulin pump as part of your diabetes management, it is essential to always have the following items available in case of pump failure and ensure that they remain on your repeat prescription:
- Back-up insulin pens for both quick acting insulin and background insulin (make sure these are in date)
- Needles for your insulin pens
A copy of your latest pump settings (in case you need to transition back onto insulin pens)In addition, please ensure that you have the following items (in date) at home and on your repeat prescription in case you are unwell, your glucose levels are running high for a period of time or have a severe episode of hypoglycaemia:
- Blood ketone meter
- In date blood ketone strips
- A copy of the sick day rules
- Diabetes pump team emergency contact details (page 2)
- Glucagon injection kit (in date – stored in fridge)
Finally, please check your pump regularly for any cracks or damage and report to your pump company if you have any issues. The company should offer a replacement for broken/damaged pumps if your pump is still within its 4 year warranty period. Pumps are replaced every 4 years providing funding requirements are met. If your pump upgrade is deferred due to unmet requirements the team will provide guidance on what to do should your pump fail.
Diabetes pump team contact numbers
Please contact the pump team if you need advice regarding your diabetes.
If you have a problem, please do not hesitate to contact us. You can leave a voicemail on one of the numbers below (the answerphone is checked regularly Mon-Fri office hours) or alternatively email.
For non-urgent queries you can message the Diabetes Educators on MyChart or email the diabetes team (these are checked Mon, Wed, Fri).
- DSN office 01223 348790
- Dietitian office 01223 348769
Urgent advice: In an emergency
If you are feeling ill or have an emergency diabetes or pump problem out of hours, contact the Type 1 Emergency Out of Hours (Mon-Fri 4pm to 11pm and 6am to 9am, weekends and bank holidays 6am to 11pm)
Telephone Service on
01223 960993
or attend your nearest accident and emergency department.
Funding requirements
Your pump and pump therapy is funded by your local Integrated Care Board (ICB). Insulin pump therapy costs over 4 times the amount of injection therapy and so you will appreciate the need to ensure that it continues to be the right therapy for you.
In order to secure ongoing funding from your ICB to purchase a new pump, we have an obligation to ensure that the pump is achieving the goal for which it was started. This is usually measured by an improvement in your HbA1c and/or a reduction in hypoglycaemic episodes.
We also need to demonstrate to the ICB that you engage in your pump therapy. This is measured by your regular attendance to clinic appointments, keeping in touch with the pump team and using your pump appropriately.
We would need to have a form of contact yearly either in person at a clinic appointment or over phone or email. Our appointment system is changing with plans to offer you a medical appointment every 18 months and a pump appointment every year if required but otherwise contact through email or MyChart initiated by yourself if support or a review is required. This is referred to as patient initiated follow up.
In situations where we can’t demonstrate an improvement, we may defer your pump upgrade in order to provide time to work with you to improve outcomes. We usually discuss upgrades a few months before your upgrade is due in order to try and provide the support in a timely manner.
Ordering supplies
Generally, we place orders on behalf of all our Medtronic pump patients automatically every 6 months as outlined below:
- We estimate what you might use over a 6 month period and this becomes your ‘regular’ order.
- The week before your order is due to be placed you will receive an email from us that invites you to make changes, if any, to your ‘regular’ order depending on current stock levels
- If you get down to a half box of remaining supply and you haven't received the pre-order notification email from the insulin pump orders team, please feel free to check in with them to find out when the next order is due to be placed
- The order will be delivered to an address of your choice (home, work, neighbour, etc). We can request delivery on a week day that is preferable to you. For example if you’re always at home on a Friday then we will request delivery to your home address on a Friday.
- If you are running out of stock we can bring orders forward for you and if you find you have too much stock we cancel the next order. If you need anything else, for example some extra supplies to go on holiday with then we can arrange this for you.
- The insulin pump orders team will, where possible, keep you informed when an order is due, placed and dispatched.
Please let the insulin pump order team know if your address and/or GP practice changes via the following email address: add-tr.InsulinpumpOrdersCUH@nhs.net
Welcome to your new pump
The basics of how an insulin pump works
Insulin pump therapy offers the closest insulin delivery system to the way the body would produce insulin without diabetes. An insulin pump uses only quick acting insulin; it delivers it in small pulses continuously throughout the day to meet your background insulin requirements; this is called basal insulin. The insulin pump can then be used to give a bolus of insulin on top of the basal insulin to cover carbohydrate eaten or give a correction for a high glucose reading.
When starting on an insulin pump, your educator will calculate your starting settings. Over a few weeks we will work closely with you to adjust your settings to suit your daily insulin requirements.
Non-urgent advice: Important information
Insulin pumps provide clever technology to better manage glucose levels, but the basics remain important. These include:
- Accurate carbohydrate counting
- Entering all carbohydrates eaten into the pump (except hypo treatment)
- Timing of the mealtime/snack insulin – a bolus given 10-15 minutes before eating is recommended
- Regular set changes
- Rotation of infusion sites
- Optimal hypo treatment
- Adjustments for activity
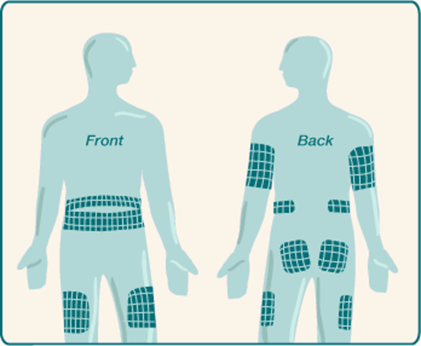
Changing the cannula sites (set change)
Remember to rotate your injection sites
It is very important to change the cannula regularly (every 2 days for steel cannulas and every 3 days for teflon cannulas) to avoid the risk of developing an infected or damaged site which can lead to poor insulin absorption
Ideally it is recommended that the set change is completed before breakfast or lunch as this provides an opportunity to check the set is working and effectively delivering insulin. The concern about changing a cannula in the evening is that it could fail and you may not be aware of this problem overnight.
Below are some guidelines to ensure your set changes run ‘smoothly’.
- Choose a time of day to change your cannula when you will need a bolus soon after the change.
- Wash your hands.
- Check your glucose level.
- Complete the set change.
- Ensure the cannula is working well:
If eating: Check your glucose level 3 hours after the set change.
If not eating: Check your glucose level 1 hour after the set change. - If glucose levels have risen further, consider doing another set change.
- After completing a second set change, return to step 5.
Reviewing your basal rate
For most people, basal rates vary across the day, and can change with time depending on changes in lifestyle or work. It can take time to work out the right basal rate, but it is important to spend time doing this, as well as checking it every so often, as the amount of insulin that your body needs changes all the time. You may find that you need to check more often if you have a change of job and especially if a work day is very different to a non-work day, or if you are going through a particularly stressful period or you have changed your activity levels such as taking up a new exercise regimen.
It is important to ensure your basal rates are correct before you look to make changes to bolus or correction insulin.
The theory is, if your basal rate is right then you could go all day without eating and your glucose would remain more or less the same!
How does it work?
An insulin pump allows you to program varying basal rates over 24 hours. Some pumps allow you to change the amount of insulin delivered every 30 minutes – that could add up to 48 different rates in one day, but most people only need about 4 to 6 different rates per day.
Remember: due to the action of quick acting insulin and the way it is delivered by the pump, a change in your basal rate will take effect 90-120 minutes later. For example, the basal rate set at midday will take effect between 1pm and 2pm.
See the following table for a step by step guide on checking your basal rates:
Non-urgent advice: Recommendations for checking your basal rates:
- We would suggest starting with your overnight basal rates
- We would suggest doing these checks a few times on days that are similar to ensure there is a pattern before you make any changes
- Ideally your glucose level at the start of each check should be between 5 and 10 mmol/L (up to 12 mmol/L can work)
- Choose a day to basal check when you;
- Have not had a hypo of 3.5 mmol/L or below in the past 12 hours
- Have not been significantly more active than normal
- Have not been unwell or are under more stress than usual
- Have not had a significant amount of alcohol in past 12-24 hours
- Abandon if you have a hypo or if your glucose levels go above 12 mmol/L and correct
| Time Frame | What to do |
When to check glucose if not wearing a sensor |
|---|---|---|
| Time Frame Overnight check |
What to do
Begin review if pre bed glucose is between 5-10 mmol/L Eat an evening meal that contains 50g or less carbohydrate that you are confident you will count accurately No food or carb containing drinks during the evening No exercise |
When to check glucose if not wearing a sensor 3-4 hours after evening meal Bedtime (if not the same time as above) 2-3am Waking |
| Time Frame Morning check |
What to do
Begin review if pre-breakfast glucose is between 5-10 mmol/L Skip breakfast Eat no food until lunch |
When to check glucose if not wearing a sensor On waking and every 2 hours until lunch |
| Time Frame Afternoon check |
What to do
Begin review if pre-lunch glucose is between 5-10 mmol/L Eat a breakfast that contains 50g or less carbohydrate that you are confident you will count accurately Skip lunch No food or carb containing drinks until evening meal |
When to check glucose if not wearing a sensor 3-4 hours after breakfast Then every 2 hours until evening meal |
| Time Frame Evening check |
What to do
Begin review if pre-dinner glucose is between 5-10 mmol/L Eat a lunch that contains 50g or less carbohydrate that you are confident you will count accurately No evening meal or carb containing drinks Eat a late snack if needed |
When to check glucose if not wearing a sensor 3-4 hours after lunch Every 2 hours until your late snack |
If the glucose levels rise or fall more than 2 mmol/L during the review period this can suggest the basal rates need adjustment.
Adjust the basal rate for the time period 90 – 120 minutes before and up to when the rise or fall in glucose occurs.
Adjust the basal rate by 10-20% or by 0.025, 0.05 or 0.10 units/hr either up or down depending on whether your glucose rose or fell.
Bolus insulin and carbohydrate counting
All carbohydrates consumed should be covered with an insulin bolus unless you are treating a hypo or being more active. The amount of insulin required is calculated by your pump when you enter the carbohydrate in grams into the bolus calculator. If you choose to miss a meal or eat a meal that doesn’t contain carbohydrate you do not need to give a bolus of insulin unless your glucose level is raised at the time of the meal.
You may find that if you have several snacks and insulin boluses in a row, the insulin can build up in the body and work more strongly than intended leading to a low reading later (insulin stacking). If you notice that this is a pattern, please speak to your pump educator.
It is important to count your carbohydrates as accurately as possible. You may find the Carbs and Cals book/app (Chris Cheyette) useful with carbohydrate counting – image shown below. We also offer Carbohydrate Counting Workshops on a regular basis. Please ask your educator to add your name to the list if you feel this would be helpful.
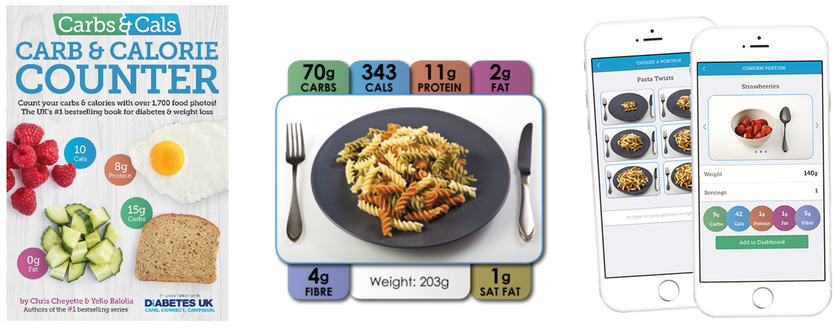

Reviewing your carbohydrate ratios
It is important to ensure your basal rates are correct before you look to make changes to bolus or correction insulin.
Your carbohydrate/bolus ratio determines the amount of insulin needed for carbohydrate eaten at a specific time of the day. In time your bolus ratios are likely to vary across the day. It is useful to be able to check if these are correct.
NOTE: choose a day to do this check when you have not been unwell, stressed, had a hypo in the last 6-12 hours, been significantly more active than usual or been drinking alcohol in the last 12-24 hours.
- Check your glucose level pre-meal. You should not have given an insulin bolus within the last 4 hours before this meal.
- Choose a simple meal that you can accurately count the carbohydrates.
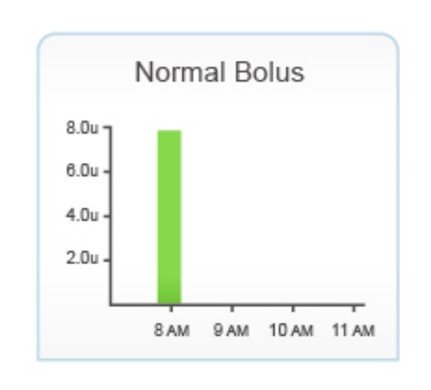
- Aim to eat less than 50g carbohydrate or give less than 6 units of insulin so that a normal wave can be used during the check.
- Give your usual insulin to carbohydrate bolus.
- Check your glucose level at 2 and 4 hours after the start of the meal.
| Timing | Target post meal glucose |
|---|---|
| Timing 2 hour post meal glucose | Target post meal glucose Within 2.8 mmol/L of pre-meal glucose |
| Timing 4 hour post meal glucose | Target post meal glucose Within 1.7 mmol/L of pre-meal glucose |
If the glucose level is out of target, review your insulin to carbohydrate ratio:
- If the glucose level rises higher than these levels increase the insulin dose by decreasing the carbohydrate ratio by 10-20% or by 0.5 to 1g
- If the glucose levels drop after a meal then reduce the insulin given by increasing the carbohydrate ratio by 10-20% or 0.5 to 1g
If at any stage during the process your glucose level drops below 4 mmol/L, abandon and have a snack. Repeat the process at another time to confirm the result.
Examples of how to change your ratio following a bolus check
Current insulin: carbohydrate ratio = 1unit:15g
Pre-meal glucose = 5.5 mmol/L, 2 hours post meal = 10 mmol/L
Increase the amount of bolus insulin by reducing the carbohydrate part of the ratio by 10-20% to 1unit:14g or 1unit:13g
Repeat the process to check whether the change was appropriate.
Current insulin : carbohydrate ratio = 1unit:8g
Pre-meal glucose = 6.3 mmol/L, 2 hours post meal = 4.1 mmol/L
Reduce the amount of bolus insulin given by increasing the carbohydrate part of the ratio by 10-20% to 1unit:9g or 1unit:10g
Repeat the process to check whether the change was appropriate
Note: The lower the carbohydrate ratio the more insulin the pump will deliver to cover carbs. The higher the carbohydrate ratio the less insulin the pump will deliver to cover carbs.
Hypoglycaemia (hypo) or low glucose level
Pump therapy has been shown to improve glycaemic control without increasing the frequency of hypoglycaemia.
It is important to note that signs of hypo may change whilst on a pump; they can become more subtle.
The important thing to remember is to recognise when you are low and treat hypos as quickly and effectively as possible.
- It is important to share this information on correct hypo treatment with close family and friends so that they can assist you, if necessary, to treat a hypo safely.
- Remember to carry quick acting carbohydrate with you at all times for treating hypoglycaemia.
- Please contact your educator if you are having frequent, unexplained hypoglycaemia (more than 2-3 per week) or an episode of severe hypoglycaemia.
How to manage glucose levels which are below target but not hypo
Pre meal/snack:
When you enter a glucose level below target before eating your pump will deduct some insulin from the meal bolus to allow glucose level to rise back into target range. You may choose to give the bolus at the start rather than 10 minutes before.
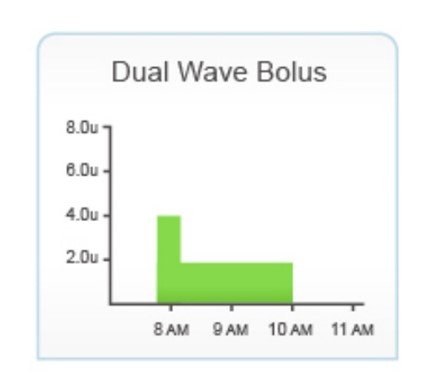
If it is a large meal or high in fat it will take longer to digest so you may wish to split the bolus and deliver half at the start of the meal and the remaining half halfway through the meal.
In between meals:
Have a small carbohydrate snack to raise your glucose to an appropriate level without covering with insulin.
For example 5g of carbohydrates will raise your glucose level by 1-2 mmol/L, 10g by 2-3 mmol/L.
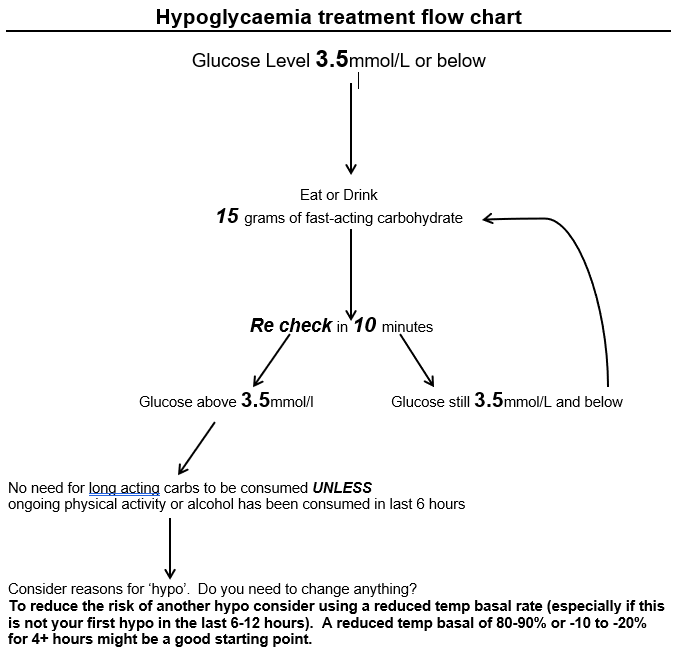
It is recommended not to correct a high glucose within 6 hours following a hypo and you may have to manually override your bolus dose to achieve this.
Severe hypoglycaemia
Severe hypoglycaemia is classified as a hypo requiring someone else to help you treat the low glucose level i.e. you would not have been able to manage on your own.
Examples include:
- A family member recognising your hypo when you have missed it and helps you to treat it
- An unconscious hypo requiring a GlugaGen® injection
Urgent advice: Severe hypo - When to call
Please call the diabetes out of hours (Mon-Fri 4pm to 11pm and 6am to 9am, weekends and bank holidays 6am to 11pm) emergency number on 01223 960993 if you (or your relative/carer) require support during or following a severe hypo.
Hyperglycaemia
Occasional highs are not thought to cause significant harm, though they can be frustrating. If you see a pattern with high glucose levels you may benefit from doing a basal or bolus review to identify a possible cause.
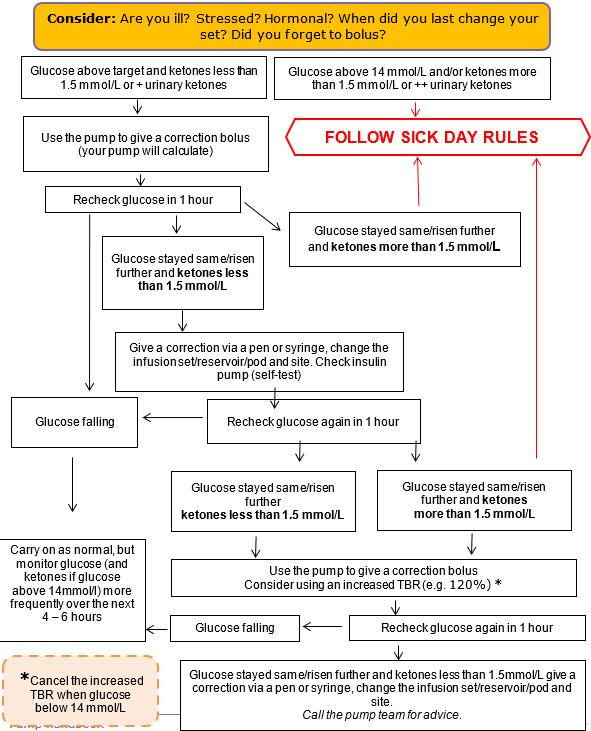
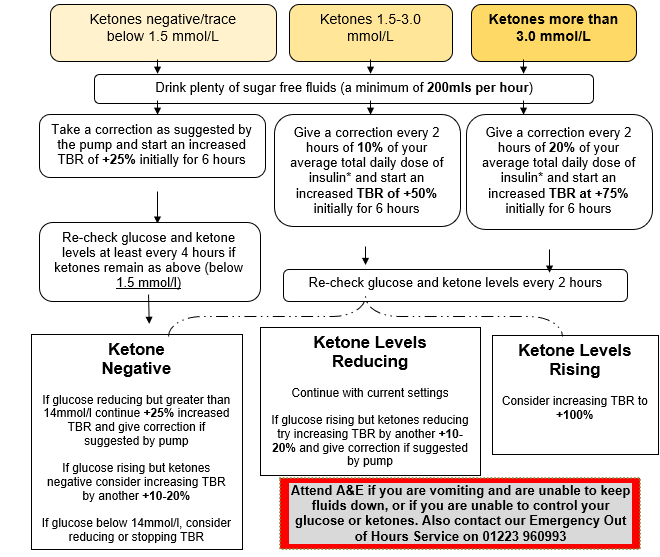
Sick day rules and diabetic ketoacidosis (DKA)
A sudden onset of high glucose levels could become life threatening if not treated quickly.
There are two common causes of rapid onset hyperglycaemia / DKA.
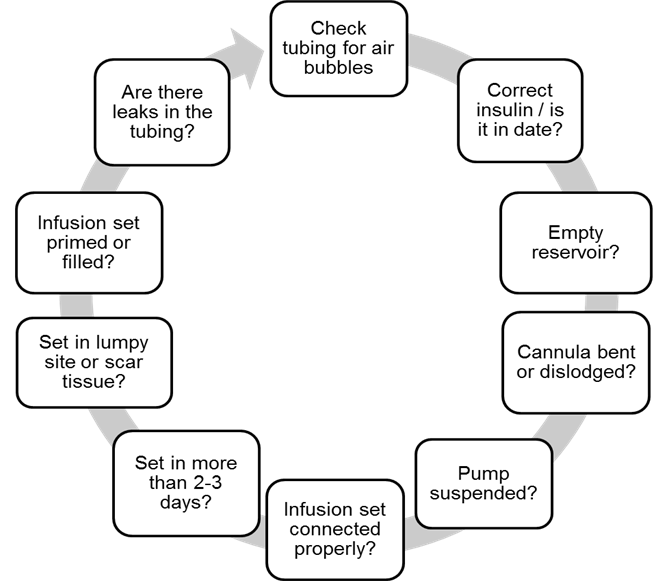
- Pump/set failure
- Illness
Monitoring your glucose levels frequently allows you to detect any significant changes in your glucose and therefore respond quickly.
When you are unwell, it is likely that your glucose levels will run higher because you become insulin resistant (caused by stress hormones) and need more insulin than normal. This response may occur even before you notice that you are unwell.
Insufficient insulin means the body cannot use glucose for energy and so fat is used as an alternative source. This breakdown of fat produces ketones and if the body cannot dispose of these ketones quickly enough they can build up in the blood to a harmful level. This is known as DKA and if left untreated, this can progress to coma or even death.
People using an insulin pump are more at risk of DKA in the event of a pump failure or failed cannula/set (because a pump uses quick acting insulin which is only active for 4 hours).
Medicines
Tablet medications often contain very small amounts of lactose but will not significantly impact glucose levels (usually <2g of lactose per day). Most liquid medications are available in a sugar free form but some liquids may contain significant amounts of sugar. A single dose of sugar containing medications is unlikely to significantly impact glucose levels. Discuss the availability of sugar free medicines with your pharmacist (including over-the-counter medication).
Physical activity and exercise
Now that you are on your insulin pump, you will hopefully find activity and exercise can be more easily managed because you can be a lot more creative and flexible with the way the insulin is delivered. Unfortunately, there is no one strategy that will work for everyone so it does require you to monitor your glucose levels and try to spot patterns in how your glucose levels react to the activities you do. In time, and with a bit of practice, it will hopefully work well for you but do use your insulin pump educator for support as it can be challenging to get right.
If you exercise regularly and/or to a high level then you may like to ask the team for the ‘Managing Exercise on an Insulin Pump’ guide for more detailed advice.
The first step in understanding how to best manage physical activity is to try to figure out how your body responds to it. Do your glucose levels drop when you’re active or in some situations do your glucose levels rise? Understanding this part will help you determine how to set the pump to cope with this.
For all activity, it is considered safe to exercise with glucose levels between 7-15 mmol/L and monitor closely. If you have ketones above 1.5 mmol/L then you should absolutely not exercise but refer to the pump sick day rules. If you have a trace of ketones (0.6-1.5 mmol/L) then you should restrict your exercise to less than 30 minutes of gentle activity.
When out and about
We would encourage you to inform friends, colleagues and family members that you are using an insulin pump and have Type 1 diabetes. There is no need to teach them how to use the pump BUT it is important to tell them what to do in an emergency, and where to find spare supplies.
Travel
You may find the link on the Medtronic website helpful to provide tips for managing travel. Traveling with an Insulin Pump | Medtronic (medtronicdiabetes.com) (opens in a new tab)
Ahead of travelling contact the pump team for a travel letter to support you carrying your insulin pump supplies, sharps and liquids through security. The pump team will arrange this letter free of charge. Please contact us, if possible, 2 weeks prior to your departure.
Insulin pumps can be damaged by being passed through certain types of security screening devices in airports such as X-ray machines and whole body scanners. Airport security staff should provide users of insulin pumps with suitable safe screening options.
Check with your pump manufacturer for guidance about flying with your pump.
If you are travelling to a hot/very cold climate or will be staying at altitude contact your pump team for support as you are likely to need adjustments to your settings.
Remember to change the time on the pump when you reach your destination as well as when you return to the UK. For very long haul travel e.g. to Australia, it may be worthwhile making small changes to the time every 6 hours.
Travel can be very stressful and therefore you may need to run an increased temp basal to ensure your glucose levels are stable. Check glucose levels frequently and correct where necessary. Also remember to drink plenty of fluid.
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/