Introduction
This information leaflet is for patients considering a Percutaneous Endoscopic Gastrostomy Tube (PEG). This may take place as a day case procedure, while you are an inpatient or may require a short hospital admission. Your healthcare team will explain what is involved and answer any questions you may have.
What is a gastrostomy tube?
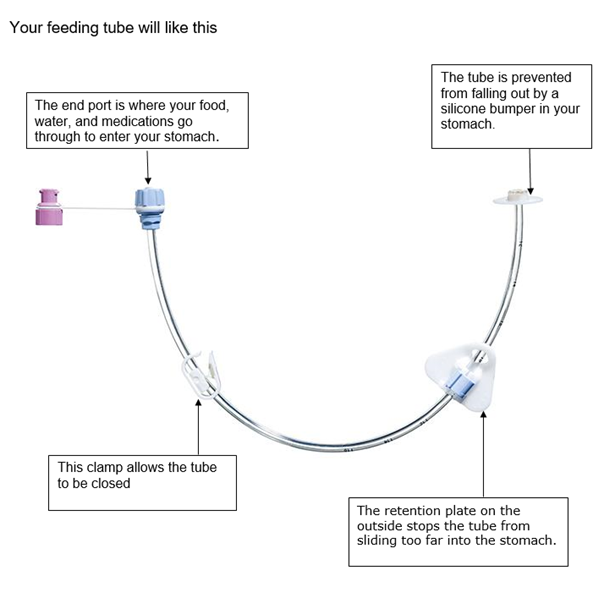
It is a tube which is placed directly into the stomach. It is also known as a ‘PEG’, which stands for:
- percutaneous (through the skin)
- endoscopic (instrument used to examine the stomach)
- gastrostomy (opening into the stomach)
Why do I need a gastrostomy tube?
Due to your medical condition, you may be unable to take enough food and/or drinks by mouth to meet your nutritional requirements. This may be due to:
- Difficulty swallowing (dysphagia) that arises from changes to the function of muscles involved in swallowing. These changes can increase the risk of food and/ or drinks to your lungs, which can result in a chest infection called aspiration pneumonia.
- Changes to your appetite and/or ability to take food orally due to reduced physical function
A gastrostomy tube can help as it bypasses the need to swallow, meaning nutrition and/or medications can be delivered directly into your stomach.
Can I still eat and drink?
Some individuals may choose to continue eating and/or drinking alongside their gastrostomy tube. If you are experiencing dysphagia, your speech and language therapist will assess your swallowing and help you to be able to do this.
How long will I need to stay in hospital to have a gastrostomy tube placed?
Gastrostomy insertion is usually performed as a day-case procedure in the Endoscopy Unit. You will be required to stay in the Endoscopy recovery area for four (4) hours where you will be closely monitored. The nutrition nurses will teach you and/or your family how to look after the feeding tube if you have not had pre-insertion training. The PEG will be flushed before you are discharged. You will be required to stay in the Endoscopy recovery area for four (4) hours where you will be closely monitored and 50mls of sterile water will be given through the PEG before you are discharged.
- If any strong (opioid) analgesia is given during the recovery period, you will need to be collected upon discharge as you will not be able to drive.
If you are discharged within 72 hours of having your PEG placed and you notice any of the following symptoms. DO NOT PUT anything through the PEG. Contact your GP (in working hours), Call 111 for advice or go to your nearest Accident and Emergency urgently.
- Leakage of fluid around the PEG tube
- Pain on feeding or flushing with water (stop the feed).
- Prolonged or severe pain with possible abdominal bloating.
- New bleeding from the PEG site
How to look after Gastrostomy tube?
It is important not to move or release the outside bumper (triangle or disc) for the first 7 days. Keeping it in place helps the site to heal.
- For the first week: Day 1 – Day 7 after the PEG insertion
- Remove the gauze dressing the day after your tube is inserted. If it feels stuck, moisten slightly with warm water to help removal.
- Apply a small amount of Octenisan antimicrobial wash neat (do not dilute in water) to a cleaning pad or gauze.
- Carefully clean around the PEG site starting at the area closest to the tube moving outward in a circular motion.
- Repeat this action (step 3) as above, using applying Octenisan if required.
- Clean the top and underside of the bumper (triangle or disc) as well
- This should be left for 1 minute before rinsing the skin around the PEG tube and the external bumper using a clean pad moistened with warm water.
- Dry around skin and bumper (including the underside)
- Apply a pea size amount of the Mupirocin (alternative Naseptin) antimicrobial ointment in the area around where the tube exits the skin.
- Secure the PEG tube to your abdomen with tape to prevent it being pulled or dislodged. This also prevents traction on the stoma.
Can I have a bath?
- For the first two days after your tube is placed do not have a bath or shower. Instead wash using a flannel with the Octenisan antimicrobial wash.
- After Day 2 you may have a brief shower or bath. Do not soak or immerse the PEG tube and exit site in water if having a bath.
- From day 8 onward if the skin around your site is clean and dry, you may return to your normal bathing routine.
If you have any concerns, please contact either your feeding company nurse or the nutrition nurse specialists.
After the first week: From Day 8 onward
It is no longer necessary to use the Octenisan antimicrobial wash and the Mupirocin Ointment, but you will need to continue cleaning the PEG site daily with warm soapy water.
You can now move the outside bumper along the tube to make cleaning the site easier. Make sure you replace the bumper approximately 2mm from the skin so that the tube does not slide in and out the stoma tract.
How to care for the Freka PEG (Advance and Rotate)
- Do not rotate the tube if the site is discharging or has not healed
- Contact the Nutrition Nurses if you have any concerns
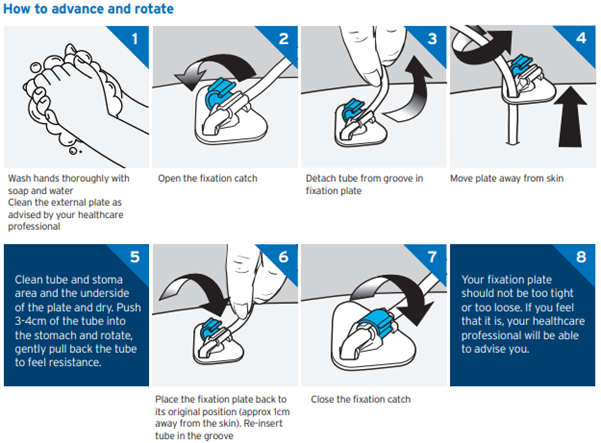
It is very important to advance and rotate the Freka PEG tube regularly. This is to prevent the internal disc getting buried in the stomach lining, a condition called Buried Bumper Syndrome. To complete this following the steps below:
- Wash your hands with soap and water.
- Release the triangular plate by opening the blue clip, remove the tube from the groove and slide back the triangular plate away from the skin.
- Clean the PEG tube, the triangle (top and underside) and skin around stoma area with warm soapy water, then water.
- Dry your skin and triangle plate (top and underside)
- Push 3-4cm of the tube into the stomach then turn the tube in a complete circle (rotate) with your fingers.
- Gently pull the tube back until resistance is felt.
- Place the triangular plate close to the skin, reinsert the tubing into the groove then close the fixation catch carefully.
- Secure the tube to your abdomen using tape or a fixation device.
What nutrition (feed) is put through the tube?
Your Dietitian will discuss specialised liquid food (feed) that is designed to provide your body with the nutrients (carbohydrates, protein, fats, minerals and vitamins) that your body needs. They will also create a plan for you that will explain how much feed you need and when to have it. It is strongly recommended that only prescribed/approved feed, fluid and liquid medications are put through the tube to avoid damage and blockages.
When should I flush my PEG tube
It is important to flush your tube to prevent blockages.
When to Flush:
- Before and after each feed or medication.
- Between each individual medication dose.
- At least once daily if not feeding, typically every 4-6 hours.
Equipment Needed:
- 60ml enteral syringe
- Freshly drawn tap water
Step-by-Step Flushing:
Position: Maintain an upright position (at least 30-45 degrees) when using the PEG tube for administration of feed, medication or water flushed. Remain upright 30 minutes to an hour after flushing or feeding to prevent reflux.
- Wash your hands with soap and water, dry then assemble your equipment
- Prepare: Draw the recommended amount of water into the syringe from a clean cup.
- Connect: Close the clamp (if available) on your PEG tube, open the cap from your PEG tube, attach the syringe, then re-open the clamp
- Flush: Slowly press the plunger, using a "push-pause" technique, pausing briefly every 5mL to push water through until complete
- Disconnect: Close the clamp on the tube before removing the syringe, close the cap then open the clamp (if available).
- Secure the PEG tubing to your abdomen with tape to prevent traction.
Cleanliness: Rinse the syringe with warm water and store in a clean container after use. Syringes can be re-used up to 1 week then will need to be changed.
How long will my tube last?
- The Freka PEG tubes that are well cared for can last for up to five years. One way of increasing the life of your tube is to leave the clamp undone when the end connector is in place. This prevents the clamp squashing the tube.
- Clamp Management: Move the clamp location up or down the tube periodically to prevent damage and prolong tube life.
What problems might I encounter after placement of a gastrostomy tube?
Pain
The site where the tube enters the stomach can be painful for a few days after the procedure. Patients are usually encouraged to use pain killers (analgesia) regularly for the first two to three days following insertion. This will be discussed this with you on the day of your procedure and painkillers prescribed if required.
Infection at the site of insertion
This can occur if the PEG site is not kept clean and dry but is rarely serious. You will be provided with a PEG treatment kit containing Octenisan antimicrobial wash and Mupirocin antimicrobial ointment to clean the PEG insertion site for the first seven days. After this period patients are usually encouraged to clean with soap and water then dry well. Dressings are not usually required.
Leakage around the gastrostomy site
Occasionally feed or gastric (stomach) fluid may leak around the tube – this commonly occurs if the triangle plate or circular disc is not close to the skin allowing the tube to slide in and out of the stomach causing leakage. This can be corrected by tightening the retention plate (external bumper) close to the skin. The surrounding skin should be cleaned and kept dry. A protective skin barrier spray maybe applied to resolve any redness/ skin irritation caused by the leakage. In exceptional circumstances, the tube may need to be replaced or repositioned at a different site.
Over granulation at the gastrostomy site
This is the appearance of light red or deep pink flesh that forms beyond the surface of the stoma opening. There are many reasons this may develop, and the treatment plans will be patient specific.
PEG tube related problems
Blockage of the tube
This can usually occur after giving some medications or not flushing the tube at the end of a feed. Though blockages can be resolved, you are encouraged to prevent this by flushing before and immediately after feed. Additional advice will be provided if you will be giving medications down the PEG tube.
Buried Bumper
This occurs if the feeding tube is persistently secured too tight against the abdomen. The internal disc can become partially or completely embedded in the stomach wall lining. This can cause leakage and infection at the PEG site and would require an endoscopy to release and replace the feeding tube. To prevent this from happening it is necessary to complete the PEG tube insertion at least once per week. Contact your Nutrition Nurse or Dietitian if you have difficulty inserting your tube.
Split or fracture in the tube
This can usually be repaired by trimming the tube just beyond the damage area and placing a new feeding end. Damage closer to the triangle would require a tube replacement in Endoscopy.
Who to contact about what?
You will be trained in all the necessary techniques to look after the feeding tube and what to do if you do have problems. However, your community nurses, GP, dietitian, and nutrition nurse will be available to help and support you. Your dietitian or nutrition team will provide regular follow up. The company delivering your feed also has a nurse helpline.
1. If you have any concerns about your feed or plastics order (including syringes and dressings) – contact your feed company:
- Nutricia Homeward: 0800 093 3672
- Abbott Hospital to Home: 0800 0183799
- Fresenius Kabi: 0808 100 1990
2. If you have any concerns about your PEG site or feeding pump – contact your feed company:
- Nutricia: 0800 093 3672
- Abbott: 0800 0183799
- Fresenius Kabi: 0808 100 1990
3. Please contact your local dietitian if you have any concerns about:
- any symptoms that suggest you are not tolerating your feed e.g. bloating, nausea
- your weight
- the amount or type of feed you take
- or if you need extra syringes or other supplies ordering
- or you want to discuss tube removal
4. Contact details for Enteral Nutrition Nurse Specialists
Monday – Friday (8am –4pm) excluding weekends and Bank Holidays
- Phone: 01223 216 037 Option 1 for Enteral Nutrition
- Mobile: 07710 365156
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

