About nasojejunal (NJ) tubes
This information leaflet is for patients who are considering a Nasojejunal tube or being discharged home with a Nasojejunal tube for the purpose of enteral feeding in community. This can be inserted during your inpatient stay or can be done as an outpatient. If an admission is required your healthcare team will explain what is involved and answer any questions you may have.
What is a nasojejunal tube?
A nasojejunal (NJ) tube is a soft tube which goes down your nose, passes through your stomach and ends in a part of your small bowel called the jejunum. This allows food and water to enter your small bowel directly where it will be absorbed. This tube is inserted in Endoscopy but can also be placed during surgery.
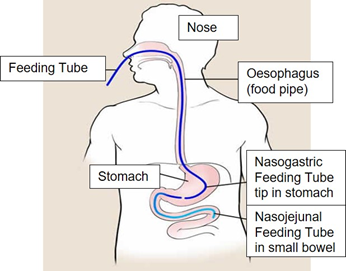
Why do I need a Nasojejunal Tube
Your medical condition may mean that you are unable to take in enough food and/or drinks by mouth to meet your nutritional requirements. This may be due to:
- Difficulty swallowing due to recent surgery, a medical condition or disease (causing an obstruction in your oesophagus or stomach), dysphagia that arises from changes to the function of muscles involved in swallowing
- Changes to your appetite and/or ability to take food orally due to reduced physical function or treatment
- You are unable to eat and drink due to illness, surgery or trauma.
A nasojejunal tube provides an effective way of providing nutrition and hydration (medications where clinically appropriate)
How long will I need to have the Nasojejunal Tube
How long you will need the tube will depend upon the reason why you have it. You will be regularly reviewed by a hospital or community dietitian who will advise you about this.
How often will tube need to be replaced?
How long your NJ will last will depend on the type used. The nasojejunal tube can be used for up to three months, at which point we recommend a routine replacement if enteral feeding is still required.
The Nasojejunal tube will need to be replaced sooner if any of the following occur
- You are unable to resolve (clear) a blockage
- You are experiencing frequent occlusion causing missed feeds or delays starting your feed
- Your feeding tube is showing signs of deterioration, for example cracks, changes in colour or stiffness when flushing.
How does the tube stay in place?
The NJ is secured with small dressings to your nose, cheek and neck. It is important to use a dressing to prevent the tube from moving or being accidently pulled out. If the dressing on your nose becomes loose, there are measurements (numbers) along the tube which you will need to check to tell if it has moved.
How often should I change the dressings
We recommend changing the dressings securing your feeding tube at least once per week or if it becomes loose.
- Remove the tape securing the tube at your nose first but leave the cheek dressing in place so that the tube does not fall out.
- Gently clean your nose and the outer area around your nostril with warm water and a mild soap.
- Pat your nose and around your nostril well to dry
- Check the outer area your nostril for any swelling, bruising, bloody, breaks in the skin or change in colour before applying new tape.
- Remove the cheek dressing
- Gently clean your cheek with warm water and a mild soap. Observe for any skin irritation (redness) or rash before replacing the dressing.
- Avoid pulling the tube tightly when securing to your cheek as this can cause pressure damage (skin to break) at your nostril
If you have any concerns about your skin integrity or dressing irritation, please contact your Community Nutrition Nurse in the first instance for advice.
Flushing
The tube can easily become blocked so requires frequent flushing with cooled, boiled water every four (4) to six (6) hours if not in use.
The NJ tube must be flushed to maintain patency and prevent tube blockage
- Before connecting a feed
- Immediately upon completion of a feed
- Every four hours with sterile water for patients who are on a build-up regime or a feeding rate which is less than 50mls per hour
- Before and after each medication and between each medication if more than one medication is given at the same time.
- When on a continuous feed every 4 -6 hours or at the change of feed every 4 hours
If the NJ tube is not being used for feed or medication, it must still be flushed with sterile water every 4-6 hours
While the NJ tube is not in use the end should be closed with the cap which is attached to the tube. This reduces the risk of infection.
Regular Mouth Care
Mouth care is very important if you are not eating. Plaque can build up quickly, so it is important to brush teeth at least twice daily. Check your mouth and throat for dryness, redness or any other abnormalities. Report any concerns to your Dietitian, GP or your managing team if you are still attending the hospital for treatment.
Medication
If you need to use your feeding tube for medication the pharmacist will need to check that it is ok to administer these down a NJ tube.
If you are prescribed medications, it is important to remind your Doctor and Pharmacist that you are using an NJ tube for administration so that the medications are provided in the right preparation for this route.
To avoid blocking feeding tubes, thick liquids should be diluted with equal amounts of water before administering.
Do not mix medications together.
Please check that if you are dispersing tablets that these can be crushed or dissolved in water before administering and that the medication is completely dissolved to prevent blocking of the tube.
Tablets that are enteric coated or state that they are sustained, prolonged or modified release must not be crushed.
What should I do if my tube falls out?
If your dressings become loose or the tube is accidentally pulled, it is possible for the tube to come out. You will require an Endoscopy to replace the NJ tube. Please contact your Dietitians or the nutrition nurse specialists for advice regarding replacement.
If you are completely reliant on the NJ tube for nutrition, hydration and medication your Dietitian may recommend an admission while you await your tube replacement
What should I do if I have nausea or vomiting when on feed?
If you experience any of the symptoms below this maybe a sign that the tip of your NJ tube has moved back into your stomach if
- Vomiting
- Abdominal distension
- Pain when feeding
- Aspiration of feed
Please contact your company nurse who can come and check the position of the tube. You can also contact your dietitian or the nutrition nurse specialists for advice within working hours. If the tube has moved back into your stomach, it will probably have to be replaced.
What to do if the tube gets blocked?
Prevention is always best. After each feed or medication, it is important to immediately flush the NJ tube with cooled boiled water to prevent the tube from blocking.
- Massage the tube between your fingers to mechanically dislodge debris.
- Start by using an empty 60ml enteral feeding syringe and apply a push /pull technique to try and release the blockage.
- You can also try this with an empty 20ml syringe
3. If this is unsuccessful, try using sodium bicarbonate solution:
- Using a teaspoon (5ml) of sodium bicarbonate powder, add to half a hot water (150ml) so that it fizzes.
- Stir well to ensure the powder dissolves then allow to cool to a warm temperature before drawing up in a 5-10mls in a 60ml syringe.
- Leave the solution for at least 1 hour then try to flush with 20ml water.
4. If the tube is still blocked change using a 60ml syringe, then try using a 20ml enteral feeding syringe following the above steps.
If these actions fail to unblock the tube, never use excessive force or attempt to insert objects (such as wire) down the tube to unblock it. Do not administer hot water through the tube to release blockage.
Contact your Dietitian or Nutrition Nurse to arrange a replacement.
Who to contact about what?
You will be trained in all the necessary techniques to look after the feeding tube and what to do if you do have problems. However, your community nurses, GP, dietitian and nutrition nurse will be available to help and support you. Your dietitian will provide regular follow up. The company delivering your feed also has a nurse helpline.
For concerns about your feed delivery or plastics order (including syringes and dressings)
- Nutricia Homeward 0800 0933674
- Abbott Hospital to Home 0800 0183799
- Fresenius Kabi 0808 1001990
For concerns about your feeding tube or feeding pump
The community nutrition nurse
- Nutricia: 03457 623672
- Abbott: 0800 0183799
- Fresenius Kabi: 0808 100 1990
Please contact your local dietitian if you have any concerns about:
- Any symptoms that suggest you are not tolerating your feed, such as bloating or nausea.
- Your weight
- The amount or type of feed you take
- If you want to discuss tube removal
Contact details for Enteral Nutrition Nurse Specialists
Monday – Friday (8am –4pm) excluding weekends and Bank Holidays
- Phone: 01223 216037 Option 1 for Enteral Nutrition
- Mobile: 07710 365156
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

