Please read, and share with your Community Nurse during visits
This leaflet is for patients who have undergone breast surgery and who are returning home with a wound drain in place. The information provided is intended to support self-management of the wound drain at home, and enable patients to seek further assistance if required.
Why do I need a wound drain?
After surgery your body will naturally produce a liquid called ‘serous fluid’ at the surgical site. If this fluid is allowed to build up under your skin it can form a ‘seroma’. This can cause swelling and discomfort and may become infected. A wound drain removes the liquid and prevents it building up.
What is a wound drain?
A wound drain is a thin plastic tube that has one end placed under your skin in the area where you have had surgery. The other end of the tube, which is outside your body, is attached to a container. The container will provide a gentle suction to draw excess fluid away, and the fluid will collect in the container.
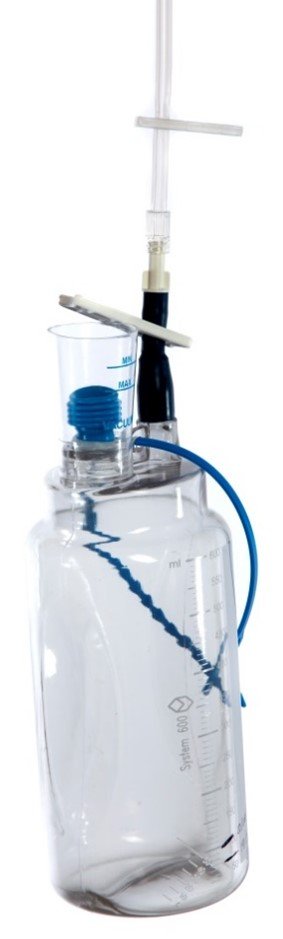
Following discharge from hospital what should you expect?
Following surgery you will have one or two drains in place, which are draining your wound of blood and tissue fluids that are produced by the body as part of the healing process. If your surgeon is satisfied with your recovery and your situation at home allows, you can be discharged with your drain in place.
For how long will I need to wear my drain?
Your drain(s) will normally stay in place for approximately 5-7 days, but this could be longer or shorter depending on how much fluid is draining each day and the type of surgery you have had.
Before you are discharged from hospital, a plan will have been put in place for the removal of the drain. This usually takes place once the fluid collected is within an agreed daily amount. Usually, we arrange to have the drain removed at the Cambridge Breast Unit.
Who will manage my drain?
The drain you have been given is suitable for you to self-manage at home. A member of the breast nursing team will make contact with you on the next working day following your discharge. They will discuss with you about monitoring the fluid output of your drain. Please raise any issues you may be experiencing with your drain to the breast nursing team. This leaflet also details common issues you may experience with your drain, how to resolve them yourself, and when / where to seek help.
Measuring fluid output from your drain
We ask you to check how much fluid is draining into your wound drain container. We have provided a table (“Fluid Output Log”) so you can record the fluid level daily.
You should measure the fluid level each morning at a time that is convenient for you. It is best to try and do the measurements at approximately the same time each day.
Method 1: Marking the container
- Mark a line on the bottle to show the level of the fluid.
- M ite the date and time next to each mark.M

Method 2: Using the Fluid Output Log
- Write down the date and time.
- Read the fluid level indicated by the scale on the bottle.
- Note the fluid level in the provided table

| Drain 1 (ml) | Drain 2 (ml) | ||
|---|---|---|---|
| Day 1 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Day 2 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Day 3 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Day 4 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Drain 1 (ml) | Drain 2 (ml) | ||
| Day 5 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Drain 1 (ml) | Drain 2 (ml) | ||
| Day 6 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Drain 1 (ml) | Drain 2 (ml) | ||
| Day 7 |
Date: Time: |
Drain 1 (ml) | Drain 2 (ml) |
| Drain 1 (ml) | Drain 2 (ml) |
Quick check: when should I change the bottle?
There are two reasons why your drainage bottle may need to be changed:
1. The bottle is full / nearly full or too heavy for you to comfortably carry
AND / OR
2. The blue indicator on the bottle is fully expanded, which shows that there is no suction left and that the drain is not able to remove fluid
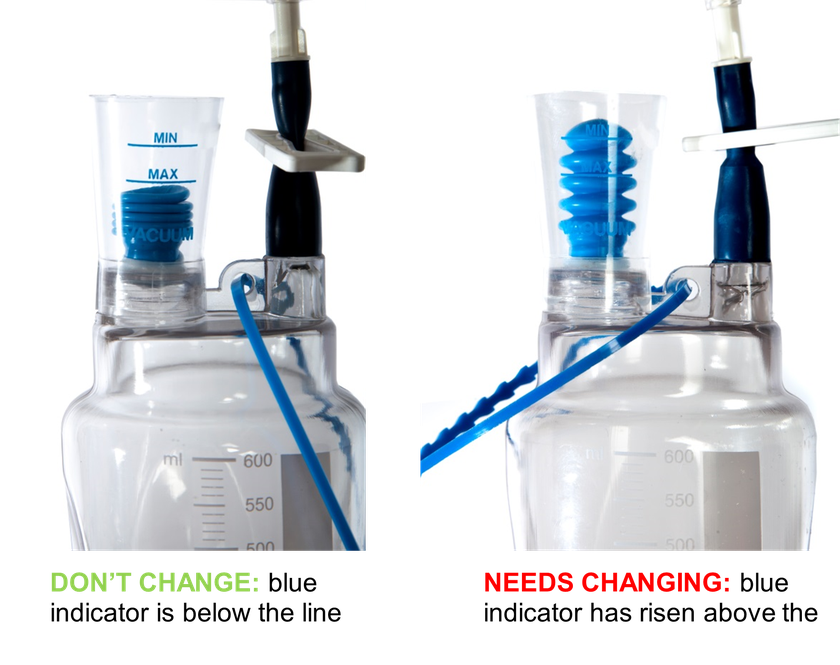
- If your Van Straten - Low Vacuum Wound Drainage System is full please change the bottle following this guide. If you do not have a spare bottle, or do not feel comfortable changing it yourself, please contact Cambridge Breast Unit. This can wait until the next working day.
- If your Van Straten - Low Vacuum Wound Drainage System bottle loses suction please change the bottle following this guide. If you do not have a spare bottle, or do not feel comfortable changing it yourself, please contact Cambridge Breast Unit. This can wait until the next working day.

Possible problems
If the following problems occur, please do not panic. Just follow the advice below:
- If the drain falls out, do not panic. It is not an urgent problem. Cover the incision where the drain leaves the skin with gauze. Use gauze or an absorbent dressing to soak up any drainage. Seek further advice by calling Cambridge Breast Unit. Please do not dispose of any part of the drain until you have received further advice.
- If your tubing becomes disconnected anywhere, place the gauze pad provided over the tube coming from the operation area, secure it with tape and contact Cambridge Breast Unit for advice. Please do not dispose of any part of the drain until you have received further advice.
- If the drain tube has been pulled out of the wound so that some of the holes in the tube show, please contact the Cambridge Breast Unit for advice. Please do not dispose of any part of the drain until you have received further advice.
- If you have excess leakage from the area where the drain comes from, cover it with the gauze pad, secure with some tape and Cambridge Breast Unit for advice.
The Breast Care Nurses can be contacted through the Cambridge Breast Unit, Monday to Friday, between 08:00 and 17:00. Should any of the above issues arise outside of these hours and you feel unable to manage, you may contact NHS 111 or, as a last resort, attend the Emergency Department.
- If you are concerned about any redness, heat, swelling, bruising and / or pain that you may have, please Cambridge Breast Unit for advice. If they are not available, please contact 111, or as a last resort attend the Emergency Department.
- If the colour of the fluid is changing, this is normal. It will change from red to pink and then yellow. Usually, the fluid will have very little odour.
How to change the bottle
If you have a spare bottle, you are welcome to change the bottle yourself following this guide. However, if you do not have a spare bottle, or do not feel comfortable changing it yourself, please contact Cambridge Breast Unit.
- Wash your hands thoroughly with soap and water.
- Close both the clip on the blue tubing at the top of the bottle attached to your drain AND the clear tubing on your drain.
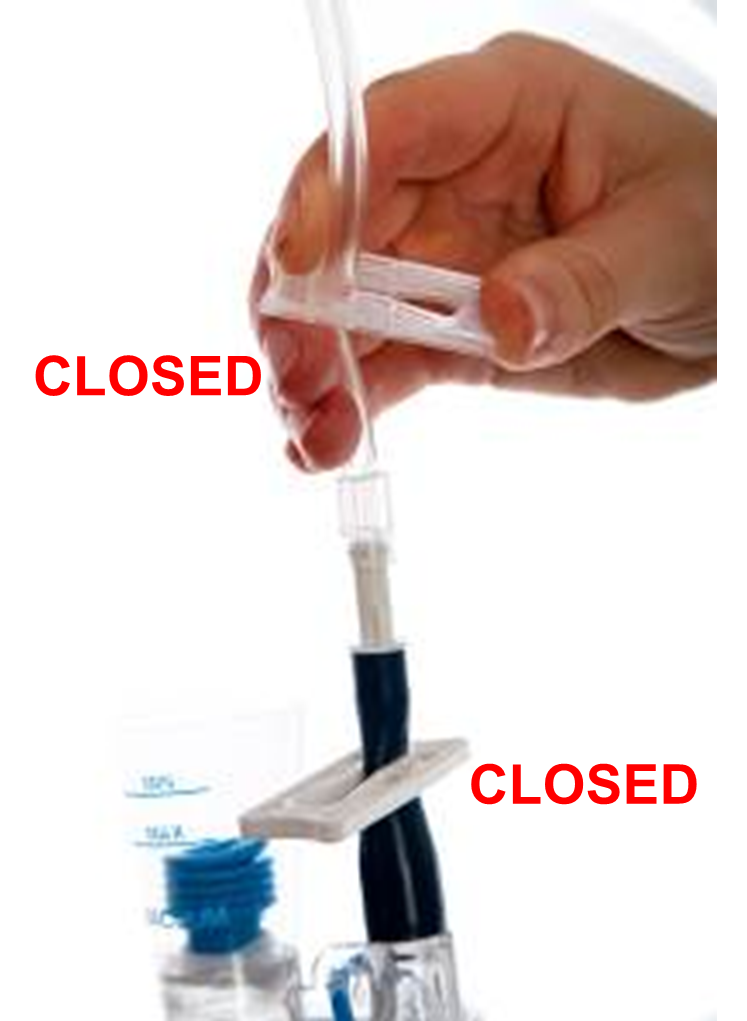
3. Disconnect the tube from the bottle by unscrewing the connector.

4. Screw on the new bottle. Make sure it is firmly attached as loose connections can lead to loss of suction. Do not release any clips before new bottle is fully connected.
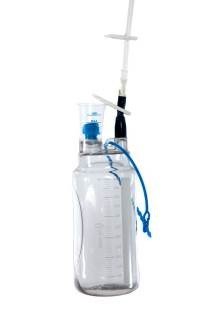
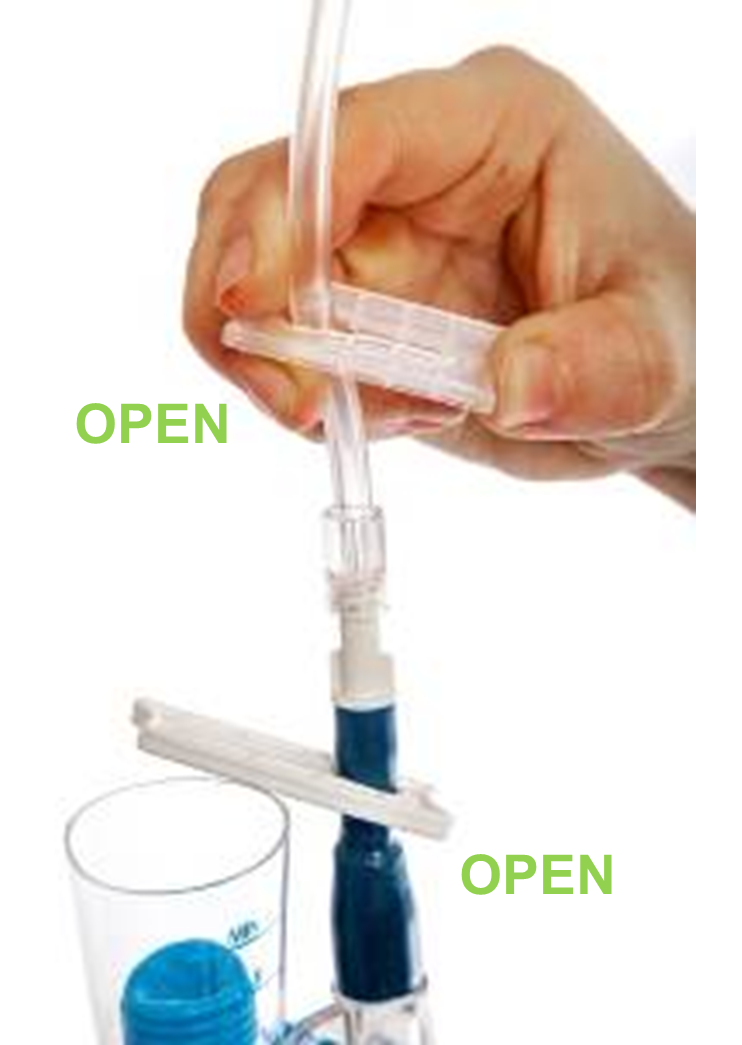
5. Open the clip on the clear tubing, AND open the clip on the blue tubing at the top of the new bottle. The new bottle is now ready to be used.
6. Store the used bottle, and take it back to the hospital when you come in for your next appointment.
7. Wash your hands.
NOTE: Closed vs Open clip positions

Contacts / Further information
For information regarding your care please contact:
Cambridge Breast Unit, Breast Care Nurses 01223 348272
For information regarding the leaflet design or publication, please contact:
Clinical Engineering Innovation 01223 216719
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

