How you choose to feed your baby and what works best for you is a unique choice for all families. The way you feed your baby may also change over time. On the neonatal unit, your baby might be given your breast milk, donated breast milk, different types of formula, or a combination of these depending on their needs. Some babies need to be given special nutrition directly into their veins. Others need to be fed by tube into their tummy until they are ready to feed by mouth.
Breastfeeding has many important benefits for both you and your baby and is particularly important for premature infants. Breastfeeding should always be considered as the first choice to feed a baby, and the neonatal staff are committed to supporting you with establishing breastfeeding. However, we recognise that there are situations when breastfeeding is not possible and also that how you feed your baby is your personal choice.
If you choose to bottle feed expressed breastmilk (EBM) and/or formula, we encourage you to continue to enjoy skin-to-skin cuddles with your baby and the benefits this brings. We will support you in learning how to :
- maintain your milk supply if you would like to combine breast / bottle feeding, or mix feed EBM / formula
- store and prepare expressed breast milk safely
- sterilise feeding equipment once home
- make up formula
- choose the best bottle for your baby's needs
Please scan the QR code to find out more about preparing infant formula and sterilising feeding equipment at home.

When can my baby begin bottle feeding?
Your baby needs to be at least 34 weeks gestation before they are ready to try bottle feeding. This is when they start to be able to coordinate sucking, swallowing and breathing. However, every baby is unique, so we also need to wait until your baby is:
- on low flow nasal cannula oxygen, or off oxygen completely
- able to keep a stable heart rate and not have increased work of breathing when being handled or with daily cares
- is not needing to be suctioned (so is swallowing their own saliva)
- can comfortably manage an amount of milk in their tummy (ie is on bolus rather than continuous feeds)
- is beginning to wake at around the time their tube feed is "due" and is able to stay awake for 5-10 minutes
- is telling you they are hungry by bringing their fists to their mouth, rooting against the mattress, poking out their tongue or crying
- has a good, strong suck on a dummy or a finger
If your baby has an underlying diagnosis, additional medical needs or is struggling with any of the above milestones then a speech and language therapist (SLT) will be asked to come and assess them and provide extra support with starting bottle feeds. The SLT may prescribe a specific bottle and teat to meet your baby's needs.
Which bottle system should I buy?
Many brands claim to have a bottle shape and teat that helps a baby to latch more easily, or is more like breast feeding, to make switching from breast to bottle easier. There is no research to back up these claims.
You may have already bought bottles in preparation for your baby to start feeding by mouth. If so, please bring these into the unit so that your baby can practise with them before they go home.
Most babies will accept any shaped teat if they are ready to feed by bottle but may need some time to learn and practise. Trying lots of different teats can be confusing for babies because the milk will flow differently. If your baby is struggling to bottle feed, please ask to see a member of the infant feeding team, or a speech and language therapist (SLT). Bottle feeding difficulties are unlikely to be due to the bottle or teat shape, but there may be other helpful strategies we can suggest to help your baby bottle feed more successfully.
Which teat should we use?
The rate or speed at which the milk flows out of the teat and into the baby's mouth when they are sucking can affect how easy or difficult a baby finds feeding. Teats are normally described using levels (level 1, 2 or 3 teat), by age (newborn, 0-3 months, 3-6 months etc), or by descriptive words (slow, medium or fast flow).
When feeding, a baby needs to learn how to co-ordinate sucking, swallowing and breathing one after the other and in the right order. They repeat this pattern many times and then take a little break from sucking and swallowing to take a few extra breaths. Most term babies (born at 37 weeks gestation) will feed very effectively with the teat that comes with a newborn bottle set.
A baby who is born preterm (before 37 weeks gestation) or is born at term and needs extra care on NICU is likely to benefit from a slower flow rate. This will mean the milk only flows when the baby is actively sucking, and they are more in control of their feeding. If the milk flows too quickly, they might lose co-ordination of sucking, swallowing and breathing and become overwhelmed by the milk flow.
Signs that the flow rate is too fast for your baby include:
- holing their breath
- oxygen levels might drop (you will only notice this if they are attached to a monitor)
- dribbling or spitting milk
- pulling away from the teat
- noisy gulping
- eyebrow raising with each swallow
- looking drowsy or falling asleep suddenly
- coughing and spluttering
How should I hold my baby for bottle feeds?
Babies who are born at term usually feed well in a cradled position. Hold your baby close to your body, so that they feel safe and secure. Support them all the way along their body with your arm and help them to keep their arms and legs tucked in. Make sure your baby can see your face and talk to them reassuringly throughout the feed.
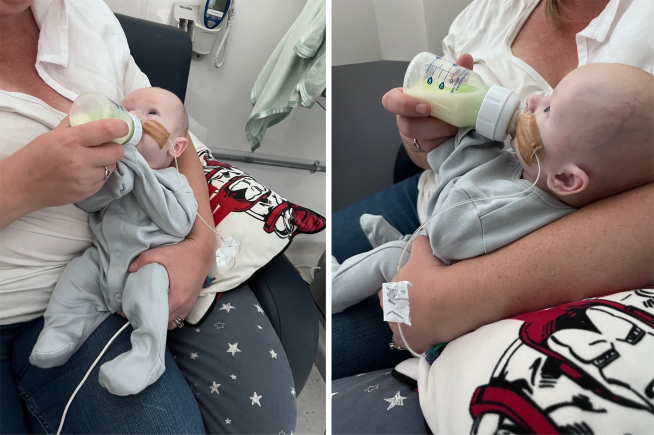
We do not recommend specific brands of bottles and teats. However, if your baby was born before 37 weeks gestation, or seems to be struggling with the flow of your current teat we would suggest searching online for the teats described as "preemie", or "extra slow flow size 0". If you do not have access to the internet or would like to discuss options further, please speak to your nurse or SLT.
| Teat description | Flow rate in mls per minute |
|---|---|
| Teat description Ultra-preemie | Flow rate in mls per minute 5 |
| Teat description Preemie | Flow rate in mls per minute 8.5 |
| Teat description Extra slow flow / size 0 | Flow rate in mls per minute 10 |
| Teat description Level 1 / newborn / slow | Flow rate in mls per minute 11-15 |
| Teat description Level 2 / 0-3 months / medium | Flow rate in mls per minute 15+ |
Once your baby is confidently finishing all of their feeds by bottle, they should be able to move on to a level 1 / newborn / slow flow teat of whichever brand you choose.
We often recommend that babies who are born preterm or needing special care are bottle fed in an elevated side lying position.
The feeder's feet are placed on step, with knees together so the baby is elevated with their head higher than their hips.
The baby is placed on their side, with hips and shoulders stacked on top of one another and bottom "sitting" on the feeders tummy.
The feeder's hand is placed on the baby's back (not behind their head) to allow the baby to pull away from the bottle when they need a break.
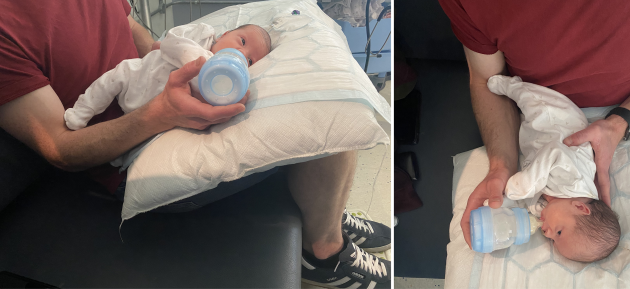
This position has many benefits:
- babies fed in this position have more stable breathing and heart rate, which means that they have more energy to focus on feeding efficiently
- offers the highest level of physical support for the baby along the whole side of their head and body, with flexion (bending) of the hips, elbows and knees
- enables self-regulation / calming strategies (baby can bring feet together, hands to midline / close to their face) slows the flow of milk
- the baby has improved control over the feed and can move on and off the teat with minimal effort. If they have too much milk in their mouth, this can safely dribble out of the side of their mouth rather than collecting at the back of their throat
- may reduce symptoms of reflux
Let your baby lead the way!
It is important that your baby is able to be in control of their feeding, and that you respond to what they are trying to tell you. Offer your baby a bottle when they tell you they are hungry (moving head and mouth around, sucking on fists). Try to feed your baby before they start to cry, as this will use up extra energy.
Watch your baby closely whilst they are feeding and talk to them during the feed. Gently rub the teat against your baby's top lip and wait for them to open their mouth, to invite the teat in.
Gently insert the teat into your baby's mouth keeping the bottle in a horizontal position (ensuring the hole in the end of the teat is covered with milk) to prevent the milk from flowing too fast.
Hold the bottle still and let your baby suck when they are ready and rest when they need to Babies need to take breaks from sucking, to catch up with their breathing. Don't be tempted to twist or jiggle the teat, to try and encourage them to suck more.
Stop as soon as your baby shows they have had enough; when their sucking slows right down or stops, or they fall asleep.
Remember that feeding is hard work and your baby needs time to build up the stamina to finish bottles. Try to focus how well the feed went and how comfortable your baby looked, rather than how much volume they took.
When can the feeding tube be taken out?
Breast or bottle feeding is the hardest work that babies have to do. It is an aerobic activity, like going to the gym! Your baby will need to build up the stamina needed for bottle feeding and will take small amounts by bottle, then have the rest down the tube. Over time, your baby will slowly start to take more milk via bottle and less by tube.
When your baby is first starting to bottle feed, they should continue to be fed every 3 hours to ensure they grow and develop. Your baby should only be offered a bottle when they wake naturally, or easily with gentle touch and voice and is showing that they are hungry. Sleep is important for recovery, growth and development, so if your baby stays fast asleep, they should be allowed to rest and fed via their tube.
As your baby progresses; is waking for most feeds, and taking the majority of their milk by bottle, you will be able to start feeding your baby more responsively (waiting until they tell you they are hungry rather than watching the clock). The feeding tube will usually be removed once your baby has taken all of the milk they need by bottle for 2 days.
Please scan this QR code to watch a Small Wonders video about moving from tube to bottle feeding:

Can we go home with the tube?
Yes; once your baby has completed 2 full breast or bottle feeds within 24 hours, you have completed your tube feeding competencies and feel confident bottle and tube feeding your baby you will be able to go home. The community team will be able to support you at home Monday – Friday, 9.00am – 5.00pm. If the tube comes out outside of those hours, you will need to bring your baby into hospital to have a new tube put in.
My Chart:
We would encourage you to sign up for MyChart. This is the electronic patient portal at Cambridge University Hospitals that enables patients to securely access parts of their health record held within the hospital's electronic patient record system (Epic). It is available via your home computer or mobile device.
More information is available on our website.
References / Sources of evidence
Privacy & dignity
Same sex bays and bathrooms are offered in all wards except critical care and theatre recovery areas where the use of high-tech equipment and/or specialist one to one care is required.
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

