Introduction
This leaflet is designed to help you and your family understand radiotherapy to renal cell cancer, especially a treatment called Stereotactic Ablative Radiotherapy (SABR). It explains how the treatment is scheduled and given, with tips on self-care during the process and after treatment. Listing common side effects doesn’t guarantee you will have them. You may also have a side effect not mentioned here. If you have any questions or concerns about the information or your treatment, please speak to a member of the team.
What is stereotactic ablative radiotherapy?
Radiotherapy uses carefully measured doses of strong x-rays to treat cancer and other conditions. It works by damaging the DNA in tumour cells causing them to die or stop growing, while allowing your normal cells to recover. SABR is an effective way of giving focused radiotherapy in fewer visits to hospital, compared to standard radiotherapy. Therapy radiographers will look after you during the planning and delivery of your treatment.
Radiotherapy itself is painless and does not make you radioactive. It is perfectly safe for you to be with other people, including children and pregnant women during the course of your treatment.
Before radiotherapy start
- Pacemaker – If you have a pacemaker, please tell your doctor or radiographer as soon as possible. We will arrange a pacemaker check before and after your treatment.
- Pregnancy – It is very important that you are not and do not become pregnant while undergoing radiotherapy planning or treatment. If you think that you may be pregnant at any point, please inform your treatment team immediately.
How is SABR given for renal cancer?
SABR for renal cancer is given as a course of one, three or five treatments, depending on the location of your cancer. These may all be completed in the same week or may be spread across two weeks. Your oncologist will tell you how many treatments you will be having.
SABR is given on weekdays with at least 40 hours between sessions. You will need to attend the radiotherapy department as an out-patient.
Most patients will need anti-sickness tablets to help with the side effects of treatment. You will be given a prescription for these from your oncologist.
These need to be taken just before your first treatment appointment.
Planning your treatment
Your case will have been discussed at a specialist multidisciplinary team meeting to ensure that radiotherapy is the best treatment option for you. You will be contacted to attend a telephone or face-to-face clinic in the hospital with your oncologist to discuss your proposed treatment. You will be asked to sign a consent for radiotherapy treatment at this appointment, or during a subsequent visit if other tests or results are needed.
If you require any additional medications to take during radiotherapy this will be explained (for example: additional pain relief medication). Finally, if we need to give you intravenous (IV) contrast (dye) for the planning scan we may need an up-to-date blood test.
The MRI and CT radiotherapy planning scans
To plan your treatment accurately, you will need a radiotherapy CT scan. This appointment will take around one hour.
The radiotherapy planning scan will take place in the radiotherapy department on Level 2 in outpatients near Oncology.
For the CT scan, you may need IV contrast to enhance the scan. If this is required, you will be asked to fill in a questionnaire and have a cannula inserted into your arm.
You may also be asked to fast before the appointment. Typically, if you are required to fast you should not eat or drink for two or three hours before your appointment. Up to 200ml of water may be sipped during this time if required - (this equates to one small cup). We recommend you have a light snack prior to fasting, for example a small sandwich or a couple of biscuits.
We will make you aware if this applies to you and will provide you with precise information depending on the specific site of your treatment.
All radiotherapy treatment is tailored to the individual patient and requires careful planning. At the CT appointment, the radiographers will position you for your radiotherapy treatment. It is important that you are comfortable lying in the planned position for up to an hour, as this will be the same position used for your radiotherapy treatment. Specific equipment may be required for scanning and treatment. This could include a custom made ‘bean bag’ to support your body (shown in image below).
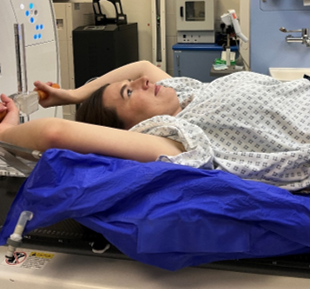
Please tell the CT radiographers, during the CT appointment, if you are uncomfortable as we may not be able to make alterations during treatment.
Your planning CT scan will have two parts. In the first part, you may be injected with contrast dye during your scan. The second part can take a little longer and will involve us placing a small box on your chest to record your breathing. This allows us to see any changes in the tumour position during your breathing cycle.
Some patients are asked to return for a second scan. This will involve wearing an abdominal compression belt. This is a piece of equipment that wraps around your abdomen and is then inflated. This is used to reduce the amount your organs move during breathing cycle. It is not painful to fit, and if used it will need to be used during every treatment.
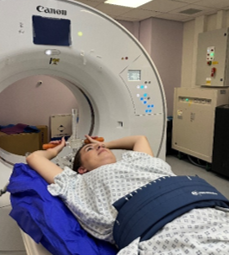
After the scan is finished the radiographers will put on some permanent small dots on your skin known as tattoos. These are used to align you in the same position for your radiotherapy treatment.
An I.D. photo and positional set-up images might be taken.
The radiotherapy treatment
Please arrive at least 20 minutes before your first appointment time as member of the team will have a chat with you to discuss the treatment and how to minimise any side effects that it may cause. They will also check that you are happy to go ahead with your treatment. This is an ideal opportunity to ask any questions that you may have. Please feel free to bring music on your mobile phone or MP3 player; this can be played through our speakers.
The radiotherapy treatment units are quite large, but they don’t touch you. Once you are correctly positioned on the treatment couch, the radiographers will leave the room to switch the machine on. You will be alone in the room during treatment, but the radiographers will be watching you on monitors. They can also speak to you via an intercom. If you need help, raise your arm. The machine can be switched off, and the radiographers can return to the room to assist you.
Scans will be taken on the treatment unit before, during and occasionally after treatments to check your position, and adjustments will be made if necessary. The treatment is then delivered. The units make a buzzing sound during radiotherapy, but it is completely painless.
There may be pauses during the procedure while the radiographers review your images or prepare the unit. A radiographer may also come back into the room part way through your treatment.
Please ensure that you remain still and in the treatment position until the radiographers inform you that the procedure has finished.
How are the appointments arranged?
We will accommodate your time preferences wherever possible. Please try to be as flexible as you can and prioritise your treatment sessions over other general appointments. The time may vary each day depending on the number of patients on the unit. Some days the radiotherapy department may be very busy, and your appointment time may be delayed. We will keep you informed of any delays. It is important to make the SABR team aware of any upcoming holiday that could interfere with the proposed treatment schedule.
What do I do if I feel unwell?
It is important that you attend each appointment. If you manage to come for your radiotherapy but feel unwell, let your radiographers know as soon as you arrive. However, if you suddenly feel unwell and are unable to come for treatment, contact your GP and the radiotherapy reception desk, who will inform your team. A plan will be put into place, and a new appointment may be arranged.
What are the side effects of treatment?
This section explains the commonly seen side effects, but this doesn’t mean that you will necessarily get them. It is also possible that you may get a side effect not mentioned here.
Early side effects of treatment
These typically peak two to three weeks after you finish your treatment and can take a further two to three weeks to reduce or settle.
Possible short-term effects from SABR are:
- Nausea and vomiting. This can happen whilst you are still coming for treatment. To help reduce this, you will be given anti-sickness medication.
- Develop discomfort in the tummy area. This is usually mild and relived with over-the-counter pain relief medication.
- You may notice that the skin around the treatment area becomes more sensitive, slightly red, warm, itchy or dry. We advise you to use mild soap and moisturiser and to avoid sun exposure to the treated area.
Please always let the radiotherapy team know if you have any worries or concerns.
Late side effects of treatment
These occur more than three months after finishing your course of treatment, but can start later.
Possible long-term side effects from SABR are:
- There is a small risk of liver and/or kidney damage. In rare cases the damage to the kidney can result in dialysis being needed.
- There is a small chance that radiotherapy will damage your bowel (gut), which may lead to a blockage in the gut, requiring an operation.
- It is possible to experience bleeding from the tumour into the kidney, which is rare but potentially serious. If you experience any flank pain, fever, vomiting or blood in your urine during or after treatment, please inform your clinical team and go to an emergency department.
Psychological effects
This information sheet deals mainly with the physical and practical aspects of your radiotherapy treatment, but the emotional wellbeing of you and your family is just as important. Having treatment can be deeply distressing for some patients. It is not unusual to feel overwhelmed by negative thoughts and feelings following a cancer diagnosis. It is important to look after yourself during and after treatment. Advice and support are always available if you are finding it difficult to cope.
There are many resources available for patients and their families and carers to cope with the emotional impact of cancer. Ask one of the treatment team or contact the Macmillan information pod, Maggie’s Centre or the Cambridge Cancer Help Centre for more information.
After treatment ends
Radiotherapy can continue to have an effect on the tumour for several weeks after treatment. The side effects from radiotherapy generally persist or worsen slightly for seven to ten days before gradually subsiding over the next two to four weeks.
Repeat prescriptions
If you need repeat prescriptions of any medication prescribed during your treatment to help with the side effects, these should be available from your GP service.
Follow up appointment
You will receive an appointment to have a follow-up with your oncologist about six weeks after treatment has finished. This may be via telephone or at the hospital. If you have not received a notification of that appointment five weeks after the end of your treatment, please telephone radiotherapy reception and ask to speak to your oncology consultant’s secretary.
Ongoing follow-up
After your six-week follow-up with the SABR team you will be referred to your original oncology team, with all information being passed onto them as well as your GP.
We do not tend to scan immediately at the end of treatment to see if the radiotherapy has worked. This is because radiotherapy continues to have an effect on the tumour for some weeks afterwards and the tumour may take time to reduce in size. Radiotherapy also causes inflammation in the surrounding tissue, meaning that X-rays and scans at that time are not so helpful.
If you are worried or notice any new symptoms between appointments, you must let your Clinical Nurse Specialist or GP know as soon as possible.
Contacts
If you have any worries or questions about any aspect of your treatment, please do not hesitate to contact one of the team.
| Service | Telephone number |
|---|---|
|
Service
Rosanna Stott Specialist SRS/SABR Radiographer |
Telephone number 01223 596329 |
| Service Radiotherapy reception | Telephone number 01223 216634 |
| Service Oncology reception | Telephone number 01223 216551/ 216552 |
| Service CUH Acute 24 hour Oncology Helpline | Telephone number 01223 274224 |
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

