Patient Name:
Patient NHS Number:
My child’s maximum Nasopharyngeal suction depths is:……cm using a size……. Fr Catheter
The maximum suction pressure is:………mmHg
On my device my suction pressure is:
Full Name: ……………………………
Designation: ……………………………
Signature: ……………………………
Date: ……………………………
Teaching Pack for Parents and Guardians
This teaching pack and associated competency document refer to children with natural airways only.
Note: If you require training to suction a child with an artificial airway please seek advice from the Tracheostomy Nursing Team or Long Term Ventilation term.
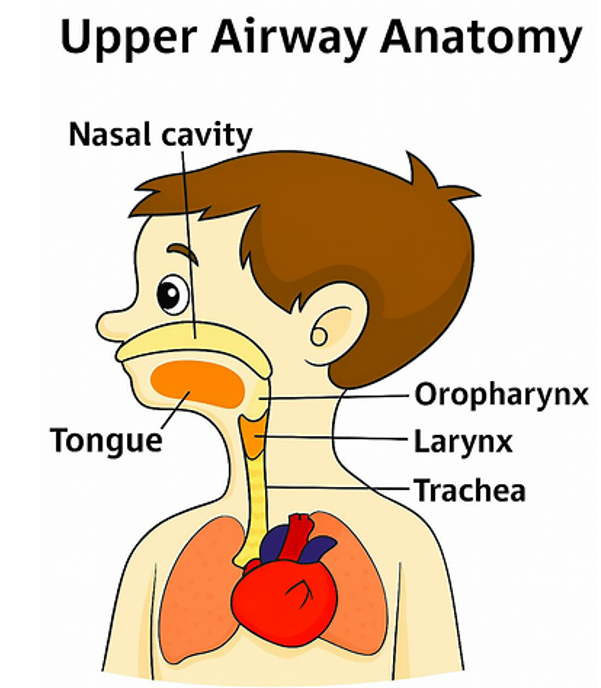
Why do we cough?
In a healthy person a cough is stimulated by secretions in the larger airways (trachea and bronchi). The body’s response is to take a deeper breath in and a forceful breath out (a cough). This is created by the diaphragm (the large muscle separating the lung cavity and the abdominal cavity) and intercostal muscles (the muscles between your ribs).
Some people do not have the strength in their muscles to create an effective cough. Others have too many secretions to be able to clear them independently. These people may require suctioning to clear the secretions in order to prevent build up in the lungs and associated chest infections.
Theory of Suctioning
Indications for suction
- Increased audible/visible secretions
- Unable to cough effectively to clear these secretions
- Decreased oxygen saturations (if measured)
- Abnormal breathing patterns
- Change in colour (for example starts to go blue around the lips)
Hazards for suction
- Increased / decreased heart rate
- Bacterial infection
- Gagging / vomiting
- Spasm along the airway
- Patient distress and discomfort
- Damage to the lining of the airway
- Fresh blood in secretions/ in mouth
- Active seizures
After suction checks
- Respiratory rate and quality
- Colour
- Heart rate
- Oxygen levels (if already being monitored)
- Quantity, colour & thickness of secretions suctioned
Suction Pressure Settings and Size of Suction Catheter
Your medical team will advise on the suction pressure and the size of suction catheter that is required for your child.
Depth of Suction
The maximum depth will have been measured by a member of your respiratory MDT this number is the furthest the suction catheter should be inserted if no cough is stimulated.
If a cough is stimulated you should not pass the catheter further than this point (Even if less than measured depth).
This depth may change as your child grows, you should speak to your respiratory team if you feel this length needs to be re assessed. You should not suction past the maximum depth as this may cause harm to your child.
Preparation
Preparation of your child
1) Explain the procedure to the child, and if they are able, ask if they are happy to continue
2) Reassure them
3) Ensure they are in a comfortable position and their airway is easily accessible
Preparation of equipment
1) Wash your hands
2) Turn on the suction switch and ensure it is at appropriate pressure
3) Ensure you have checked you have the appropriately sized catheter to hand
4) It is helpful to have a yankauer suction to clear large amounts of secretions if cleared to mouth during the procedure
Procedure
1) Connect the catheter to the suction
2) Apply glove - Do not touch anything but the catheter with this hand
3) Take the Catheter out of the packaging ensuring this touches only your sterile glove
4) Insert the catheter into the mouth to lubricate initially/ use optilube if you prefer
5) Insert the catheter into the chosen nostril and pass the catheter until cough is stimulated or the child’s designated depth is reached.
6) Place thumb over hole at the end of the catheter to apply suction and withdraw catheter
Please Note: Steps 4 – 6 (combined) should take no longer than 10 to 15 seconds.
Post-Procedure
1) Ensure your child is comfortable
2) Check the oxygen saturations (if appropriate/able)
3) Assess how hard it is for them to breathe
4) Does suction need repeating?
5) Is further help required? (see below)
6) Dispose of the used catheters and gloves. Then clean equipment as needed.
When To Seek Further Assistance
Call 999 if;
- Your child appears to be in distress (for example if they have change in colour or if their breathing is much harder or abnormal for them)
- Oxygen saturations (if monitored) remain consistently low following suction.
Contacts/Further information
For information regarding this leaflet, you can contact:
The Paediatric Physiotherapy Team
Phone: 01223256726
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

