How does it work?
Tirzepatide raises hormone levels that regulate insulin production and slow digestion, helping you feel full sooner and reducing appetite.
Importance of diet and exercise
As with all treatments for diabetes, it is important to eat a healthy, balanced diet. Make sure that you include plenty of protein in your diet, and exercise regularly, including muscle strengthening exercises, to avoid losing muscle mass whilst taking this medicine.
Possible weight loss
You may experience weight loss after starting on this medication. Losing 5-10% of your body weight can noticeably improve your blood glucose levels. You may follow the plate model below to help with weight loss:
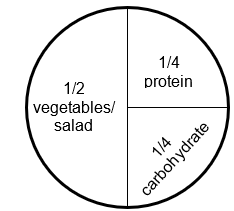
A healthy dinner plate is made up of these types of foods:
- Half the plate (50%) should have vegetables, salad or fruit.
- One-quarter of the plate (25%) should have protein, such as meat, fish, eggs, beans or lentils.
- One-quarter (25%) of your plate with wholegrain carbs like sweet potatoes, brown rice, brown pasta, or quinoa.
Importance of protein
Protein supports weight loss by promoting fullness, preserving muscle, and raising metabolism. If your appetite is low, make protein a priority at each meal. Try to choose from whole food sources and avoid processed meat such as bacon and sausages as they are high in salt and saturated fat which are not good for your cardiovascular health. Animal - based foods like pork, chicken, duck, beef, fish, eggs and dairy products, are high in protein, as are plant-based foods like beans, pulses, tofu and Quorn®. Please talk to your dietitian if you would like to know what your protein target per day is.
Snacking
Snacking in general can make it harder to manage a healthy weight which is crucial for managing your diabetes. If your appetite is reduced and you struggle to finish a full meal, go for a healthier option which contains protein and fibre. For example, 0% fat Greek yoghurt topped with fruits or a handful of nuts, boiled eggs, a glass of skimmed milk, low fat cheese, a handful of mixed nuts such as peanuts, walnuts or brazil nuts , cottage cheese, chicken breast slices, edamame / soya beans, carrot sticks and hummus.
Protein supplements
Sufficient protein requirements may be met through dietary intake. Protein supplements such as shakes and cereal bars, might be a convenient way to increase protein intake, but they do not contain the added benefits of other foods such as fibre, vitamins and minerals. High protein labels do not always mean a product is healthier or has more protein than a normal food These products may contain additional sugars, fats, and additives. Certain items might possess less or equivalent protein content by weight compared to their standard versions. Always check the full nutrition label for ingredients. If you have concerns that you are not achieving your protein targets you can consider discussing this with your healthcare team.
Be physically active
Being physically active during weight loss is important. Exercise burns calories, helps you lose more weight than diet alone, and prevents the loss of muscle and bone mass that can occur when you lose weight with diet only.
Aim for at least 150 minutes of moderate-intensity aerobic activity (like brisk walking or dancing) or 75 minutes of vigorous activity per week. Incorporate muscle-strengthening activities that work all major muscle groups on two or more days a week. Even small amounts of activity can add up and provide significant health benefits. Aim to be more active throughout the day.
Consideration of supplements
If you are not able to eat a balanced diet, you might benefit from taking certain supplements e.g. A-Z multivitamins and minerals. Keeping a food diary could be useful to track your nutritional intake. There are apps that can be used if this is helpful. Your medical team can offer personalised advice on your individual requirements.
Eat Mindfully
Since you may experience appetite suppression, it is important to recognise when you are full and stop eating accordingly. You can use the hunger scale below to help determine if you are hungry or have eaten enough.
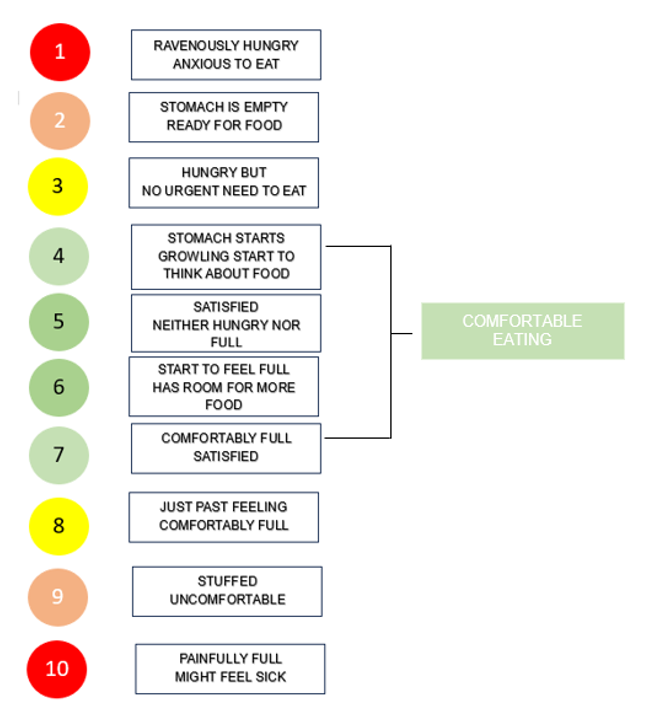
Diet tips for managing side effects
The patient information leaflet that comes with your medication has a full list of possible side effects. You are unlikely to have all the side effects listed and may not get any of them. If you do experience any side effects, make a note of them and talk to your healthcare professionals. The following management tips for side-effects of this medication may or may not work for you. If your symptoms persist or are unmanageable, please speak to your GP. Keeping a food and symptom diary may help you to identify any problem with foods that may be worsening your symptoms.
|
Possible side effects |
Consider | Avoid |
|---|---|---|
| Nausea / vomiting |
Consider
Small, frequent meals with snacks in between, because having an empty stomach can make you feel worse. Eat slowly and give your food time to settle by relaxing after meals in a sitting or slightly reclined position, instead of lying down Keep well hydrated with sugar free / low calorie drinks between meals, rather than with your food. Small amount of plain, dry foods, such as toast, crackers or plain biscuits, may help to settle your stomach Ginger tea or peppermint tea may help to settle your stomach. If you vomit, try to increase your fluid intake to replace lost fluids If you require medication to help you cope with nausea and sickness, please ensure you take this exactly as prescribed, usually about 30 minutes before eating. |
Avoid
Very sweet, spicy, fatty or fried foods Large portions of meals Strong smelling foods |
| Diarrhoea |
Consider
Drink at least 2 litres of fluid every day to avoid dehydration Have small frequent meals and snacks rather than large meals. Choose soft, easily digested foods, e.g. white fish, mashed potatoes, yoghurt etc. You might find it helpful to keep a food diary if you think certain food triggers the diarrhoea If your diarrhoea does not settle, speak to your doctor who may prescribe some antidiarrheal medication |
Avoid
High fibre foods e.g. wholegrain cereals, brown rice and pasta, beans, lentils and pulses Spicy, fried or very fatty foods, like curries, chillies, cream, pastry, chips, alcohol, strong tea or coffee, or pure fruit juice |
| Constipation |
Consider
Aim for at least 2 litres of fluid every day Aim for five portions of fruits and vegetables/day. Try a maximum of 150ml of fruit juices that are high in sorbitol e.g. apples, apricots, peaches, pears, plums and prunes. Eat 2-3 kiwis a day (including the skin) Choose wholegrain options e.g. All Bran, oat bran, brown rice, ryvita rye crispbread, seeded bread Include beans and pulses in your diet such as red kidney beans, lentils Add 1 tablespoon of flaxseed/linseed to your diet e.g. soup, salad, cereals Increase physical activity level If you are still constipated after following the above suggestions, you may wish to consider using laxatives e.g. Fybrogel, lactulose. Please consult your pharmacist. |
Avoid
Limit processed foods, sweets, white bread, and other refined carbohydrates Straining, as this can contribute to other problems When you feel the urge to have a bowel movement, go to the toilet and don't delay. Alcohol and caffeinated beverages can increase the risk of dehydration, so limit your intake. |
|
Sulphur burps (a foul rotten egg smell) |
Consider
Try green, peppermint, and chamomile tea Have small frequent meals and snacks rather than large meals |
Avoid
High-sulfur foods e.g. eggs and dairy products, cruciferous vegetables e.g. brussels sprouts, broccoli, cabbage, cauliflower, and kale Pungent vegetables such as garlic, onions, and leeks Spicy and fatty food Beer, cider and wine Fizzy drinks |
| Reflux |
Consider
Eat smaller amounts at regular intervals and avoid drinks with meals. Try not to miss meals. Relax at mealtimes. Sit up when eating and avoid sitting in a low chair with a tray on your lap. Sleep in a semi-upright position or with the head of the bed raised a few inches to help to prevent nighttime symptoms of reflux. Seek medical advice if you want to consider taking medication. |
Avoid
Having large meals. Eating late at night and ideally eat your evening meal three to four hours before going to bed Bending, lifting or lying down straight after meals Heavy exercise immediately after eating Eating on the go Alcohol Some people find the following foods may make symptoms worse: Tea or coffee, fizzy) drinks, citrus fruits and juices such as orange, grapefruit, lemon and lime, tomatoes and tomato based foods such as pasta sauces and tomato juice, spicy foods, garlic and foods containing garlic, rich/fried/fatty/greasy foods e.g. pastry, creamy sauces, rich desserts, fried batter, chocolate, vinegar |
If you have any queries please do not hesitate to contact the diabetes team via telephone on 01223 348124.
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

