This information leaflet aims to inform you about a healthy diet and lifestyle for you after your pregnancy with gestational diabetes.
To confirm the gestational diabetes has gone away it is recommended that you continue to check your glucose levels until your baby is one day old and have an HbA1c blood test three to six months after the birth. This can be done at the Rosie Hospital or at your GP surgery.
Once your baby is born
- If your gestational diabetes was treated with insulin and/or metformin tablets, this treatment should stop immediately after the birth of your baby, unless you have been advised otherwise.
- We recommend that you monitor your blood glucose levels for the first 24 hours after your baby’s birth. The targets are more relaxed than during pregnancy; aim for less than 7.0mmol/l on waking (after fasting) and below 11.1mmol/l one hour after meals. Please inform your midwife if your levels are above these targets.
- Although there is no need to keep to the strict dietary guidelines you followed during your pregnancy there is great benefit in continuing with a healthy balanced diet.
- If you were overweight before your pregnancy or gained more than the recommended healthy weight gain during your pregnancy, you will benefit from reducing your weight to a healthy weight. This will reduce your risk of developing gestational diabetes if you have another pregnancy and help to reduce your risk of developing type 2 diabetes.
Your baby will have their blood glucose monitored until they show that they are managing their own glucose at a healthy level. See Increased risk of low blood sugars after birth: information for parents
Feeding your baby
It is important you feed your baby in the way that suits you and your family best.
Colostrum harvesting
- Colostrum (early milk) is produced in your breast from around 16 weeks into your pregnancy and is rich in antibodies. It is also high in carbohydrates, which can support normal blood glucose levels.
- You can start hand-expressing colostrum from 36 weeks of pregnancy unless you have been advised otherwise.
- Colostrum packs can be collected from Clinic 21 when you come in for your 36-week scan. We will provide guidance on the technique at the late pregnancy online meeting.
- Colostrum can be used to support your baby’s glucose levels if they are low in the hours after birth or if your baby is not interested in taking a feed at that time.
Skin to skin contact
- Keeping skin-to-skin contact with your baby in the first few hours, or as long as you want to, will help to encourage regular feeding and keep your baby warm and calm, which has been shown to help keep their glucose in a healthy range.
Breastfeeding
Breast milk provides everything your baby needs up to six months of age and has many benefits beyond this time. Breastfeeding can reduce your risk of developing type 2 diabetes by up to half and/or delay a diagnosis by up to 12 years.
Contraception
It is possible to get pregnant from three weeks after giving birth even if you are breastfeeding and therefore it is helpful to think about the best form of contraception for you.
There are many contraception options available, please see links for further support:
- Family Planning Association website (opens in a new tab)
- Integrated Contraception and Sexual Health services website (opens in a new tab)
- NHS where to get contraception (opens in a new tab)
Developing gestational diabetes in future pregnancies
- If you developed gestational diabetes, it is more likely to reoccur in future pregnancies. Eating a healthy diet, achieving a healthy weight and being more physically active prior to becoming pregnant can reduce your risk of developing gestational diabetes.
- Before you start to try to conceive ask your GP for a blood test to rule out diabetes before you get pregnant.
- In your next pregnancy, please inform your community midwife at booking that you had diabetes in a previous pregnancy. To screen for gestational diabetes, we will offer you an early oral glucose tolerance test.
Developing type 2 diabetes in later life
The risk of developing type 2 diabetes can be reduced by making some healthy diet and active lifestyle changes including:
- achieving a healthy weight for height (see BMI Chart)
- following the healthy eating principles (see Healthy Eating)
- being active every day (see Start exercise)
- breastfeeding (see above)
As the risk of type 2 diabetes often runs in families, adopting these principles as a family is beneficial for you all, and can help protect future generations from diabetes. The National Diabetes Prevention Programme gives information and support on how to reduce your risk of developing type 2 diabetes. This programme is available to women who developed gestational diabetes; your GP can refer you to this or you can self-refer at Healthieryou (opens in a new tab).
Studies have also shown that women who have had diabetes in a pregnancy also have an increased risk of developing heart disease in later life, even if they do not develop type 2 diabetes. Risk of developing heart disease (opens in a new tab)
We recommend that you ask your GP each year to review your blood pressure and cholesterol levels and support you with stopping smoking, if this is an issue for you.
What is type 2 diabetes?
- Type 2 diabetes is a condition where the body is unable to regulate the level of glucose (sugar) in the blood and glucose levels can run higher than is healthy.
- Most people with type 2 diabetes have some degree of insulin resistance, where insulin does not work effectively, and they are unable to produce enough additional insulin to compensate for this.
- It is possible for glucose levels to run higher than is healthy but not so high that you feel unwell or different. This is why it is important that you are screened for type 2 diabetes every year by your GP. Some GPs will invite you for this screening, but others might not, so please check with your GP to see what their arrangement is. Some women use their baby’s birthday to remind them to book this screening appointment.
- Very high blood glucose levels can cause unpleasant symptoms, such as thirst, tiredness, increased frequency of passing urine and mood swings. If you develop these symptoms, you should see your GP as soon as possible.
- Over a long period of time, high blood glucose levels cause damage to some parts of your body including eyes, kidneys, and your heart so it is particularly important for blood glucose levels to be kept in a healthy range of 3.5 to 10.0mmol/l.
Risk factors for type 2 diabetes
Some of the risk factors associated with developing type 2 diabetes are out of your control, such as genetics. However, there are some factors which you can change to reduce your risk of developing type 2 diabetes; these include being a healthy weight, eating a healthy diet and being active every day.
The following are risk factors for type 2 diabetes:
- a member of your family has type 2 diabetes (parent, brother or sister, grandparent)
- you are above a healthy weight
- you have high blood pressure
- you have polycystic ovarian syndrome
- you have impaired glucose tolerance or impaired fasting glycaemia
- gestational diabetes in a previous pregnancy
- certain medications such as steroids or antipsychotics
The more risk factors that apply to you, the greater your risk of developing type 2 diabetes.
Reducing your risk of developing type 2 diabetes
Being a healthy weight for your height, eating a healthy diet and taking regular physical activity can reduce your risk of developing diabetes.
When can I start exercising?
It is advised that you wait until after your six-week postnatal check before resuming regular exercise. If you had a caesarean section your recovery time may be longer. For more advice, please speak with your midwife or GP. After your postnatal check at six weeks, you could join a postnatal exercise class. It may help to be with other new mums. If you plan to go to an exercise class that is not specifically for postnatal mums, please tell the person running the class if you have had a baby in the last few months. It is important that you take care of your back and avoid exercises that could injure it. Remember that any increased physical activity will be beneficial for you. This can be going for a walk with friends or family, gardening, cleaning, dancing; it does not have to be a sport.
Can I take my baby along?
Many postnatal classes let you do the exercise class with your baby at the side of the room. Some exercise classes allow the baby and pram in as part of the workout. Ask your health visitor if they know of any in your area.
Other activities you could do
It is recommended that you start your exercise off gently and feel comfortable with what you are doing. You could try the following:
- Keep up your postnatal exercises.
- Push your pram at a brisk pace, keeping your back straight. Walking is a good form of exercise, so walk as much as you can.
- Climb your stairs at a brisk pace. It is likely that you already go up and down many times a day, so think of it as good exercise!
- Squat down to pick things up from the floor, holding anything with a significant weight close to your body. This is also something you are likely to be doing a lot. If you squat rather than stoop, bending your knees and keeping your back straight, this helps to strengthen your thigh muscles and avoid damaging your back.
- When your postnatal bleeding (lochia) has stopped, you can try swimming. If you take your baby with you, try to have someone else there too so that you get a chance to swim.
- Play energetic games with older children. You can exercise by running about with them. You might be able to find outdoor space if there is no space at home.
There are free online exercise classes available. This way you can do a workout at home. You could get a friend or your older children to join in. An example is BODYFIT by Amy (opens in a new tab)
Healthy Eating
Many women report feeling much better in themselves when they followed the diet for gestational diabetes and continue with many aspects of the diet after the birth of their baby. You are encouraged to eat a healthy diet that is high in fibre, low in saturated fat, low in added sugar and low in refined carbohydrate and salt and which includes plenty of fruit and vegetables. The ’Eatwell Guide’ (below) aims to help you get the balance of foods in your diet right.
Try to choose foods from the different sections of the plate in the proportions shown below.
- 1/3 to 1/2 (a third to a half) plate of vegetables
- 1/4 to 1/3 (a quarter to a third) plate of protein
- 1/4 to 1/3 (a quarter to a third) plate of one carbohydrate
There are many benefits to eating a healthy diet including:
- feeling well
- achieving and maintaining a healthy weight
- avoiding constipation
- reducing the risk of developing heart disease and some cancers
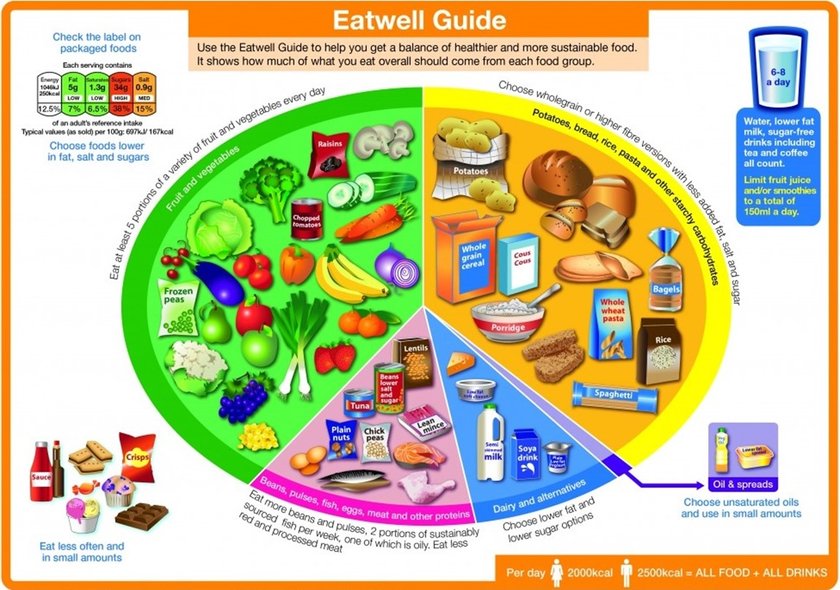
The Eat Well guide
For more information on how to eat a healthy diet please visit eatwell guide (opens in a new tab)
Food Labels
Looking at the food label and using the ‘per 100g’ numbers can help you decide whether the food product contains ‘high’ or ‘low’ amounts of fat, sugar, and salt. Try to choose ‘low’ and ‘medium’ options as guided below. Helpful link. (opens in a new tab)
|
Measure per 100g |
This is classed as ‘low’ |
This is classed as ‘medium’ |
This is classed as ‘high’ |
|---|---|---|---|
|
Measure per 100g |
This is classed as ‘low’ A healthier choice |
This is classed as ‘medium’ Ok most of the time |
This is classed as ‘high’ Just occasionally |
|
Measure per 100g Fat |
This is classed as ‘low’ 3g or less |
This is classed as ‘medium’ 3g to 17.5g |
This is classed as ‘high’ More than 17.5g |
|
Measure per 100g Saturated fat |
This is classed as ‘low’ 1.5g or less |
This is classed as ‘medium’ 1.5g to 5g |
This is classed as ‘high’ More than 5g |
|
Measure per 100g Sugar |
This is classed as ‘low’ 5g or less |
This is classed as ‘medium’ 5g to 22.5g |
This is classed as ‘high’ More than 22.5g |
|
Measure per 100g Salt |
This is classed as ‘low’ 0.3g or less |
This is classed as ‘medium’ 0.31g to 1.5g |
This is classed as ‘high’ More than 1.5g |
Fibre – aim for 3g or more per 100g and high fibre 6g per 100g
Achieving a healthy weight
Keeping your weight within the healthy range also reduces the risk of developing type 2 diabetes. You can measure if your weight is affecting your health and risk of developing diabetes by measuring your Body Mass Index (BMI). This measures your weight against your height.
A BMI of 25 and over is classed as overweight, and a BMI of 30 and over is classed as obese. Obesity, or having a BMI of 30 or more, is associated with increased health risks including type 2 diabetes and heart disease.
You can use this link to calculate your BMI (opens in a new tab) or you can use the chart below.
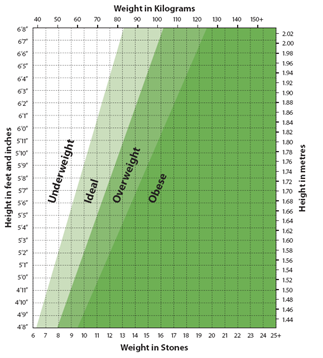
Body Mass Index (BMI) Chart
This BMI chart can be helpful as a quick guide to assessing weight in most adults.
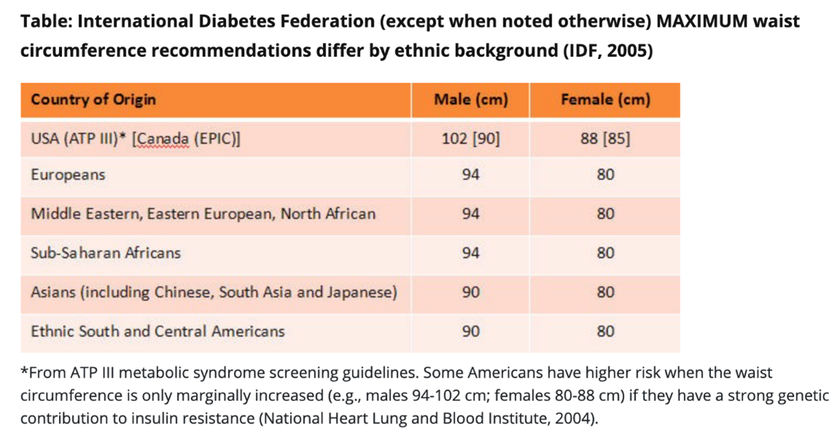
However, adults of South Asian populations living in the UK have a higher than average risk of developing heart disease and type 2 diabetes than the rest of the UK population. They are also more likely to store body fat around their middle, which further raises the risk of developing these conditions. So if you are South Asian, it is especially important to consider your waist measurement as well as your BMI. If you are not sure about how this affects you, please speak to your GP.
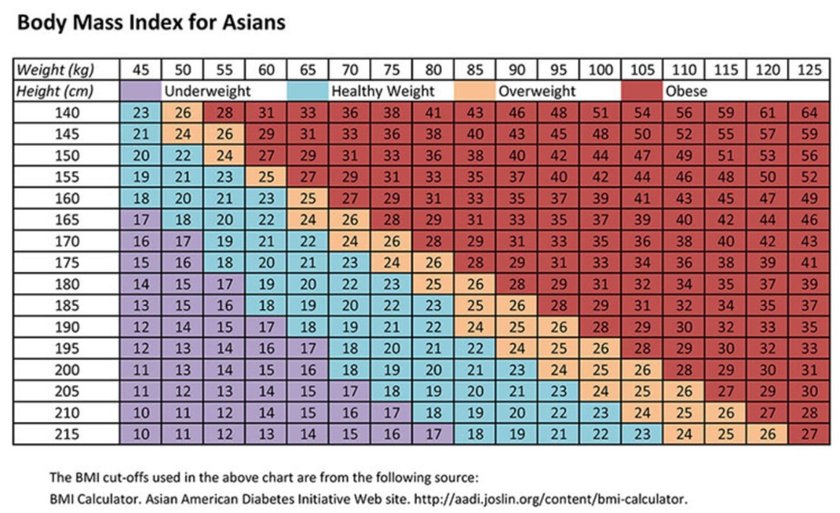
To measure your waist circumference, take a suitable tape measure and and place this on your bare abdomen between your hip bone and belly button. Relax your abdominal muscles and breathe normally. The tape measure is to be close to your skin but not pressing in and not gapping. This will enable you to use the table below to compare your own waist measurement. This table details the maximum waist circumference recommended for different countries of origin. If you find that your waist circumference is measuring above the recommended one, this is an indicator that weight loss would be beneficial for you to help reduce your risk of developing type 2 diabetes and to enhance your health. For more information about waist measurements, see heart-matters-magazine (opens in a new tab).
To lose weight, you need to use up more energy (calories) than your body takes in from food and drink.
Small changes can make a big difference
Small changes to your diet and lifestyle will have a positive impact on you and your family’s health, both now and in the future. Rather than making drastic changes that leave you feeling overwhelmed or that are too hard to keep to, why not make small changes that are simple to follow? By making small changes bit by bit, you can help to make new habits and changes that last.
- Make your change realistic and achievable; you will feel more positive and empowered as you make the change. For example:
- “I will start with a brisk 15-minute walk to the shops twice a week and then build this up to a 30-minute walk on three days and/or at a faster pace.”
When you have (perhaps) never run before, this will be more achievable than: - “I am going to run for an hour a day every day.”
- “I will start with a brisk 15-minute walk to the shops twice a week and then build this up to a 30-minute walk on three days and/or at a faster pace.”
- Plan your meals ahead and prepare a shopping list for these meals. You will then only buy the food you need and be less likely to buy extra or less suitable food.
- Avoid shopping when you are hungry, so you are less likely to make impulse buys.
- Cut down the quantity. It may sound simple, but just eating smaller portions will reduce calorie intake. Eating from a smaller plate which holds less food, and ordering small portions, are both ways that can help you to reduce the quantity you eat.
Other sources of support
Examples of local services may include:
- NHS Diabetes Prevention Programme (NHS DPP) your GP can refer you, or you can self-refer at healthieryou (opens in a new tab)
- A dietitian can offer more specialist, individualised advice to manage your weight. To access a dietitian, you will need to be referred by your GP.
- An exercise referral scheme run by exercise specialists, usually within local leisure centres. Please ask your GP if there are any in your local area that they can refer you to.
- Everyone Health is the council’s weight loss and exercise referral schemes for Cambridge residents with medical conditions such as obesity and diabetes, whose health would benefit from leading a more active lifestyle (opens in a new tab).
- Community-based schemes promoting health, such as healthy cooking sessions, healthy lifestyle clinics and walking for health programmes.
- Commercial weight loss groups such as Slimming World and Weight Watchers.
What about the rest of the family?
If you think that your children could also benefit from having a healthier diet and being more active, they may like to visit the following website: Better Health, healthier families (opens in a new tab)
Contacts and further information

Diabetes UK (opens in a new tab)
Diabetes Charity

Buggy Fit (opens in a new tab)
Fitness classes for mums

Exercise classes in your area

British Heart Foundation (opens in a new tab)
Healthy Eating Publications

Better Health, healthier families (opens in a new tab)
Phone: 0300 123 4567
Provide tips and ideas to help families eat well, keep active and search for activities in your local area.
Exercise referral schemes (opens in a new tab)
Local council’s exercise referral schemes for Cambridge residents with medical conditions such as obesity and diabetes, whose health would benefit from leading a more active lifestyle.
We are smoke-free
Smoking is not allowed anywhere on the hospital campus. For advice and support in quitting, contact your GP or the free NHS stop smoking helpline on 0800 169 0 169.
Other formats
Help accessing this information in other formats is available. To find out more about the services we provide, please visit our patient information help page (see link below) or telephone 01223 256998. www.cuh.nhs.uk/contact-us/accessible-information/
Contact us
Cambridge University Hospitals
NHS Foundation Trust
Hills Road, Cambridge
CB2 0QQ
Telephone +44 (0)1223 245151
https://www.cuh.nhs.uk/contact-us/contact-enquiries/

